Abstract
Have you ever heard about amyotrophic lateral sclerosis (ALS)? ALS, also called Lou Gehrig’s disease, is a disease that results in muscle weakness and paralysis caused by the death of nerve cells. ALS is a rare disease—approximately 60,000–380,000 people are diagnosed with ALS each year all over the world. ALS is considered an age-associated disease, as symptoms usually appear after age 50. Despite being studied for the last 100 years, the causes of ALS remain unknown, and there is still no effective treatment or cure. ALS symptoms worsen quickly, and affected individuals become entirely dependent on caretakers. People with ALS typically die within 1–3 years following diagnosis. Awareness campaigns like the Ice Bucket Challenge can raise interest in ALS and money for studying—and hopefully one day curing—this rare and terrible disease.
Lou Gehrig was an American baseball superstar! While playing for the New York Yankees in the late 1920s, Gehrig won national championships, broke records for hitting home runs, and held the longest consecutive streak of games played for over 60 years-2,130 games in a row! He was often called the “Iron Horse” for his strength, athleticism, and perseverance. However, in 1938 when Lou Gehrig was just 35 years old, fans started to notice something was amiss. He was no longer able to hit the home runs he used to, and he became clumsy and slow in his movements. Eventually, Lou Gehrig was diagnosed with early onset of a disease called amyotrophic lateral sclerosis (ALS), forcing him to retire from baseball. Sadly, he passed away 2 years later at the age of 37, and because of his struggle with this disease, ALS is also commonly called Lou Gehrig’s disease [1].
What is ALS?
In ALS, muscle cells are not controlled properly due to the breakdown of the nervous system, which normally controls our muscle movements. ALS patients progressively lose the ability to control their muscles. ALS was discovered in 1869 by Jean-Martin Charcot, but the disease became more widely known following Lou Gehrig’s death. Although ALS has been around for many years, there is still no cure. ALS is a rare disease—around 15 people per every 1 million are diagnosed with ALS each year. This means that in the U.S., which has a population of around 328,000,000, approximately 6,000 people are diagnosed with ALS each year [2].
The cause of ALS is still largely unknown. Scientists know this disease is not infectious or contagious. Sometimes it is passed down in families, but other times it is sporadic, which means random, with no clear cause. Most cases of ALS are sporadic. Although ALS is present worldwide, there is a higher prevalence in Europe. ALS affects more men than women, and generally symptoms arise between 51 and 66 years of age. The progression of ALS is rapid, with most affected individuals dying within 1–3 years after diagnosis [3]. However, this is not always the case. In approximately 1 out of 10 ALS patients, the disease progresses slowly, with survival of longer than 10 years [3]. One of the most well-known examples of slow progression is Stephen Hawking, a famous theoretical physicist who lived with ALS for over 50 years.
The nervous system
Everyday movements such as running, swimming, or eating are performed by muscles, which are controlled by signals coming from the brain. These signals travel through nerve cells (neurons), which are the building blocks for the brain and spinal cord. Together, the brain, spinal cord, and nerve cells throughout the body make up the nervous system (Figure 1A).
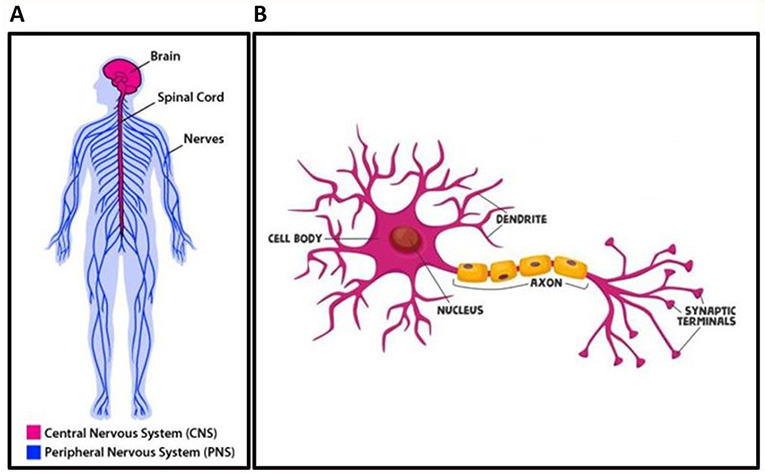
- Figure 1 - (A) Organization of the nervous system.
- The brain and spinal cord make up the central nervous system, and the nerves throughout the body make up the peripheral nervous system. (B) Structure of a neuron. The dendrites receive signals, and the axons send signals to other cells, including muscle cells.
To picture a nerve cell, imagine a tree with a short, roundish trunk (the cell body), branches (dendrites), and a long root (axon) (Figure 1B). The dendrites receive signals from other nerve cells, and the axon sends electrical signals to other nerve cells or muscle cells. The nerve-cell process of sending an electrical signal is known as signal transduction. When another neuron or muscle cell receives an electrical signal, the signal might stimulate that cell to perform an action or stop an action.
How does the nervous system function?
The brain and spinal cord are the structures that organize all the nerves. Specific areas of the human brain control specific functions of the body. For example, the left side of the brain is responsible for speech, and the front part of the brain is involved with memory. Motor neurons are a type of nerve cells that control all muscle movements in the body, with the information they get from the brain (Figure 2). When the motor neurons are damaged, which is what happens in ALS, the brain can no longer send signals to the muscles, which causes the loss of muscle function and paralysis.
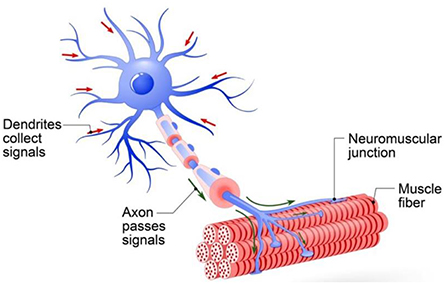
- Figure 2 - Structure of a motor neuron.
- The dendrites receive a signal from the brain and the axon passes that signal directly to the muscle cells, which causes the muscle cells to contract. This process is important for muscle function.
What are the symptoms of ALS?
There are two main types of ALS, which are categorized by their initial symptoms. The majority (80%) of patients show their first symptoms in the muscles of the arms or legs. This is called spinal onset. In the remaining 20% of ALS patients, the disease first affects muscles of the neck and head, which may cause difficulty in speaking or swallowing. This is called bulbar onset [3].
Because the motor neurons are affected, people who have ALS might have trouble with everyday activities, such as writing, tying shoelaces, dressing, walking, or climbing stairs. They may also have difficulty swallowing, speaking, or keeping their balance. Some ALS patients also show behavioral changes such as a lack of interest in what is going on around them. During the later stages of disease, difficulty breathing is another serious symptom.
The first symptoms of ALS may occur anywhere in the body. From that starting point, however, the progression is usually predictable. For example, if the muscles of the left leg are affected first, the disease will most likely affect the muscles of the right leg next, followed by the right arm, the left arm, and then finally the head and neck muscles.
What causes ALS?
We still do not know what causes ALS—YET! However, there are several risk factors that increase a person’s chance of developing the disease. These include older age (over 50), male sex, and a family history of ALS [4]. However, family history of ALS is rare among all ALS cases: only about 5–10% of all people with ALS have a familial link. Also, genetic mutations can play a part in the onset of the disease, especially for familial ALS cases. Other potential risk factors that are still being studied include lower body mass index (BMI), smoking, high blood lipid levels, eating red or processed meat, and environmental exposures such as air pollution. Individuals with several risk factors might have a higher risk of developing ALS compared with those who have only one risk factor present [3, 4].
Difficulties for caregivers
In most cases, individuals with ALS are cared for by family members, volunteers, or home nurses. These caregivers not only have to take care of the physical needs of ALS patients, including feeding and bathing them, but they must also face the emotions of watching a loved one struggle with the disease. People with ALS get sicker quickly following diagnosis—little by little, they may suffer from paralysis and inability to communicate effectively, and they are likely to die in a short period of time. Caregivers facing this situation can experience emotional distress and even mental health conditions such as anxiety or depression [5].
Conclusion
ALS is a rare disease of the motor neurons. A lot about ALS remains unknown today, but scientific research will help scientists and physicians understand the cause of ALS and eventually develop a cure. Ongoing ALS research will eventually allow scientists to identify specific risk factors and high-risk groups, to detect the disease earlier and more accurately, and to develop treatments that will prolong survival following diagnosis. Although there is still no cure for ALS, treatment options have improved over the past 20 years and hopefully will continue to do so.
Scientific research takes money. Therefore, disease-awareness campaigns, particularly those for rare diseases, are important to drive scientific discovery. The 2014 ALS Ice Bucket Challenge aimed to spread awareness of ALS and raise money for research. Challenge participants spilled buckets of ice water over their heads within 24 h of being challenged, and shared their videos on social media, where they also tagged more people to participate in the challenge and donate money (Figure 3). People who did not want to dump ice-cold water on their heads could donate money to ALS research instead—but many people both completed the challenge and donated to this important cause! The ALS Ice Bucket Challenge raised $220 million dollars for ALS research, which has accelerated scientific discovery in the past couple of years [6]. Maybe you will get the chance to participate in a future challenge, to help raise awareness and money to better understand—and hopefully cure—this deadly disease.

- Figure 3 - Members of the Department of Clinical Neuroscience at Karolinska Institutet and the Neurobiology Department at Karolinska Sjukhuset complete the ALS Ice Bucket Challenge to raise awareness for ALS.
Glossary
Amyotrophic Lateral Sclerosis (ALS): ↑ A disease that affects motor neurons in the brain and spinal cord, which results in muscle weakness and the loss of muscle control.
Neuron: ↑ Cells that make up the nervous system (brain and spinal cord). Sends and receives signals from the brain to communicate with cells throughout the body. Also called nerve cells.
Dendrite: ↑ Part of a neuron that receives cellular signals from other neurons.
Axon: ↑ The tail-like structure of a neuron that sends signals to other cells.
Signal Transduction: ↑ A chemical or physical signal that is sent within or between cells and results in a cellular response.
Motor Neuron: ↑ Cells in the brain and spinal cord that send signals to the muscles. These signals give people the ability to move, speak, swallow, breathe, and more.
Paralysis: ↑ Loss of muscular function. Often results in the inability to move certain parts of the body. For example, paralysis in the legs results in inability to walk.
Conflict of Interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Acknowledgments
Written informed consent was obtained from the individual(s) for the publication of any identifiable images or data included in this article.
References
[1] ↑ Brennan, F. 2012. The 70th anniversary of the death of Lou Gehrig. Am. J. Hospice Palliat. Med. 29:512–4. doi: 10.1177/1049909111434635
[2] ↑ Mehta, P., Kaye, W., Raymond, J., Punjani, R., Larson, T., Cohen J., et al. 2018. Prevalence of amyotrophic lateral sclerosis—United States, 2015. MMWR Morb. Mortal Wkly. Rep. 67:1285–9. doi: 10.15585/mmwr.mm6746a1
[3] ↑ Longinetti, E., and Fang, F. 2019. Epidemiology of amyotrophic lateral sclerosis: an update of recent literature. Curr. Opin. Neurol. 32:771–6. doi: 10.1097/WCO.0000000000000730
[4] ↑ Sun, J., Huang, T., Debelius, J. W., and Fang, F. 2021. Gut microbiome and amyotrophic lateral sclerosis: a systematic review of current evidence. J. Intern. Med. 290:758–88. doi: 10.1111/joim.13336
[5] ↑ Poppe, C., Koné, I., Iseli, L. M., Schweikert, K., Elger, B. S., and Wangmo, T. 2020. Differentiating needs of informal caregivers of individuals with ALS across the caregiving course: a systematic review. Amyotroph Lateral Scler Frontotemporal Degener. 21:519–41. doi: 10.1080/21678421.2020.1771735
[6] ↑ Sohn, E. 2017. Fundraising: the ice bucket challenge delivers. Nature, 550:S113–4. doi: 10.1038/550S113a
