Abstract
Eating a less-than-healthy diet can increase the chances of becoming obese, which usually happens when body organs have difficulties using or storing the excess fat and sugar that we eat. To better understand how what we eat affects the functioning of our organs, we measured substances called metabolites, which come from food, in the blood of obese minipigs. We then used computers to figure out what happens to these metabolites inside the liver following normal meals or a fast-food meal. We found that the liver fights against unhealthy food by finding ways to use or remove the excess fat and sugar. However, some of the paths normally followed by healthy food might become blocked when we eat too much unhealthy food. Our work showed that a better understanding of how the liver processes the metabolites from unhealthy diets could help people suffering from the effects of obesity.
What Is Obesity?
The fat that we eat is stored in a specific type of tissue called adipose tissue. Adipose tissue is made of cells called adipocytes, or fat cells. Stored fat comes from the fatty foods we eat, but it also comes from sugary foods because the body can convert sugar to fat. Obesity is a chronic disease, in which too much fat is stored in the adipocytes, making them grow bigger and causing the body to become fatter. Obesity eventually leads to more serious health problems, like diabetes. When too much fat or sugar is consumed, it is stored in the adipocytes, but it can also be stored in the liver. The liver is a very important organ because it is in charge of handling sugar and fat. Since the main role of the liver is not to store fat, too much fat can be toxic for this organ, making it difficult for it to work normally. This can be very dangerous for our health. Therefore, it is important to understand how the liver uses the fat and sugar we eat, especially when we consume too much junk food or too many fast-food meals.
What Is Metabolism?
All organs are fed by blood vessels, which bring them the molecules they need to function properly. These small molecules are called metabolites. Metabolites that are transported by the blood to the organs can come from the foods we eat, or they can be made by other organs. Organs use metabolites to make energy, or as building blocks to create other bigger molecules that the organs need to function. Organs can also make new metabolites and send them back to the blood, so other organs can use them. The transformations of metabolites into other metabolites are called metabolic reactions. A chain of metabolic reactions first forms a metabolic pathway, and then all these pathways form a huge “road map,” called a metabolic network (Figure 1).
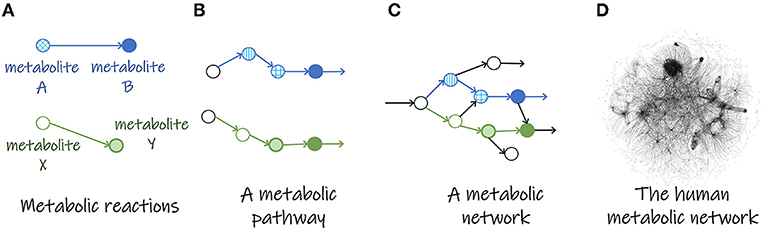
- Figure 1 - The metabolic network.
- (A) In metabolic reactions, metabolites (A or X, represented by circles) are transformed into other metabolites (B or Y), as shown by the arrows. (B) A chain of metabolic reaction forms a metabolic pathway. (C) A metabolic network is a combination of many metabolic pathways. (D) The human metabolic network illustrated here contains 13097 reactions and 10067 metabolites. (Image credit: [1], using the MetExplore webserver [2]).
The metabolic network of an organ can be compared to the road map of a city. In a city, some goods are produced in factories and then transported to shops where they can be stored and later delivered to your house. When everything works well, the shops are continuously supplied by the factories and goods can be delivered to your house whenever you need them. When a road becomes blocked by an accident or by too much traffic, there may be some delays in the delivery. Everything gets really messy when too many roads become blocked: shops might become empty and unable to deliver the goods you need. The same might happen to the metabolic network when a person becomes fat or obese: some metabolic pathways might be blocked, causing the organs struggle to do their normal work, either not making metabolites that need to be made or storing large amounts of metabolites that should be sent to other parts of the body.
In our study, we wanted to understand which paths of the liver’s metabolic network are blocked or disturbed in obese people and how this might affect their health.
Studying the Effects of Obesity on Organs
To understand how our organs deal with the fat and sugar we eat, we must use a living animal as a model. If the animal model is similar enough to the human, it can help us understand what happens in the human body. Rats and mice are the most commonly used animal models, but in our study we chose to use the minipig. The minipig is very similar to a common pig but smaller, even as an adult. Minipig organs work very similarly to human organs and minipigs also digest food in a similar way. Minipigs eat several meals each day, like humans do. Because minipigs are bigger than rats and mice, we can obtain bigger blood samples from them and take blood more often. Finally, minipigs are a very good model to study obesity because they show the same symptoms as humans [3]. To study what happens in minipigs’ organs when they become obese, we fed minipigs meals containing a lot of fat and sugar (like fast-food meals) every day for 2 months. We weighed the minipigs every week. After 2 months, we took blood samples to measure the amounts of sugar and other metabolites in the minipigs’ blood.
Computer Models Can Help Us Understand What Happens in Our Organs
To understand how an organ works, we often need to take samples from it—but this can be complicated. Instead, we took blood from the vessels that enter and leave the liver of minipigs, to study which metabolites, and how much of them, are present in the vessels. In the laboratory, hundreds of metabolites can be measured at once using a technique called metabolomics [4]. By comparing the amount of each metabolite at the entrance and exit of the liver, we can see which metabolites have been produced or used by the liver. This tells us about what is happening inside that organ (Figure 2). Then we can compare what happens in the liver under various conditions. For example, if we observe that the amount of glucose (a sugar metabolite that is the main fuel for cells) coming out of the liver is much lower in one condition than in another, it may mean that less glucose was produced in that condition. Maybe the road producing glucose was blocked, or the glucose was used to make something else (Figure 3).
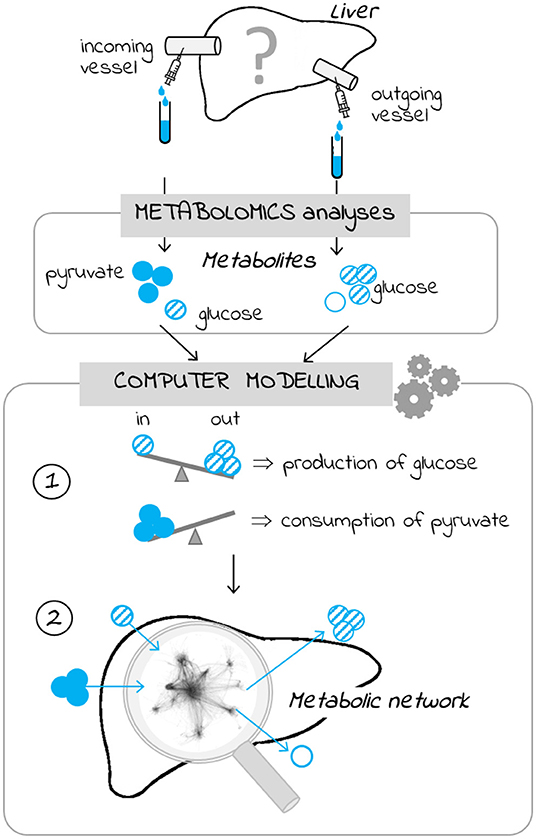
- Figure 2 - Understanding liver metabolism using metabolomics and computer modeling.
- Blood is taken from the vessels entering and leaving the liver. Metabolomics is used to see which metabolites (such as glucose and pyruvate) are present and in what quantities. We use computer modeling to figure out if the metabolites were produced or consumed by the liver (1). For example, if we measure more glucose in the outgoing vessel than in the incoming vessel, it means that glucose is produced by the liver. The computer model helps us learn about what happens inside the liver and the paths followed by various metabolites (2).
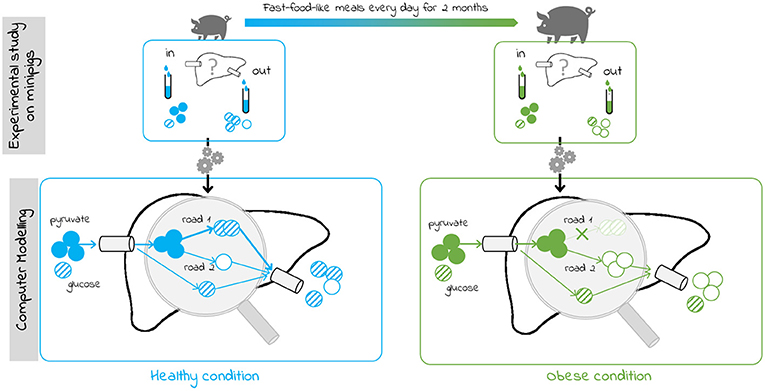
- Figure 3 - What is happening in the liver of obese minipigs?
- Our model can help to understand what happens in the liver. It searches paths that were followed by the metabolites present in the incoming vessel to obtain the metabolites present in outgoing vessels. For example, in the “healthy” condition, glucose but not pyruvate was present in the outgoing vessel, meaning that glucose was produced by the liver and pyruvate was used up. The model proposes that path 1 was used. In the “obese” condition, less glucose was present in the outgoing vessel t: the model predicts that path 2 was used instead of path 1 because path 1 might be blocked.
This kind of reasoning is easy to do for one metabolite. However, when you have hundreds of metabolites and many roads, it is too difficult for the human brain to figure out which metabolic roads are blocked. Fortunately, computers can help! In this case, the computer model is like a GPS or Google Maps: using calculations and some information about the traffic, it can help scientists figure out which roads are blocked, and which are not. In our case, computer models helped us to guess which metabolic roads were used by the metabolites, giving us new ideas about what may be happening in the liver. We could then check these ideas using other experiments.
Obesity Changes the Way Our Organs Deal With Food
After only 2 months of eating fast-food-like meals, the minipigs became obese. They stored large quantities of fat in their bodies and we also found larger amounts of sugar in their blood. Thanks to metabolomics, we identified which metabolites, and how much of them, were present at the entry and exit to the liver. With the help of computer models, we learned that, after eating fast-food for 2 months, the minipigs’ liver did not work as well as they usually did in the healthy condition.
What went wrong inside the liver? The liver of obese animals changed the way they used or produced metabolites. Also, the metabolites did not take the same “roads” inside the liver when the minipigs were obese. Using the new roads had negative consequences for the obese minipigs: their liver stored more fat and became less able to deal with fast-food meals. The liver is very important for controlling the amount of fat and sugar in the body. Therefore, if the liver does not work correctly and starts to store too much fat and sugar, it can lead to serious health complications, like diabetes. We found that, even after just 2 months of eating fast-food meals every day, the consequences for the liver were already very negative.
Conclusions
The liver is one of the most important organs in the body: it is the primary organ that tries to protect us from the bad consequences of unhealthy food. In obese minipigs, thanks to metabolomics and computer models, we figured out that when too many fast-food meals are eaten, the liver starts to use the metabolites incorrectly. These changes may push the liver to store more sugars and fats in an attempt to protect the body. Too much fat and sugar stored in the liver can have harmful consequences for other organs and disturb the way the whole body deals with fat and sugar. These changes could be the beginning of serious diseases, like diabetes. If the human liver works like the minipig’s liver, we believe that these negative consequences could also happen in humans who eat too much fast-food. This evidence supports the idea that a balanced diet, low in fat and sugar and high in fruits and vegetables, could help to keep the liver, and therefore the entire person, healthy.
Glossary
Adipose Tissue: ↑ Parts of our body which are composed mainly of adipocytes and which store fat.
Adipocytes: ↑ Cells whose main function is storing fat. They are also called fat cells.
Obesity: ↑ A disease which starts developing when too much fat is ingested and needs to be stored in the body.
Diabetes: ↑ A condition that occurs when the body can’t use sugar normally. Too much high sugar levels will eventually lead to long-term damages in multiple organs.
Metabolites: ↑ Small molecules that are directly ingested from foods or produced in the body by transforming other molecules or breaking down bigger molecules.
Metabolic Network: ↑ The complex web of relationships between metabolites, composed of many interlinked metabolic pathways.
Metabolomics: ↑ Laboratory techniques that help to identify and measure the amounts of thousands of metabolites that are present in a sample of blood or body fluid or organ.
Computer Model: ↑ A computer program that uses mathematical calculations and rules to reproduce the functioning of an organ (like the liver, in our case) and predict how things will behave under different conditions.
Conflict of Interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Original Source Articles
↑Tremblay-Franco, M., Poupin, N., Amiel, A., Canlet, C., Rémond, D., Debrauwer, L., et al. 2020. Postprandial NMR-based metabolic exchanges reflect impaired phenotypic flexibility across splanchnic organs in the obese Yucatan mini-pig.
References
[1] ↑ Robinson, J. L., Kocabaş, P., Wang, H., Cholley, P. E., Cook, D., Nilsson, A., et al. 2020. An atlas of human metabolism. Sci. Signal. 13:eaaz1482. doi: 10.1126/scisignal.aaz1482
[2] ↑ Chazalviel, M., Frainay, C., Poupin, N., Vinson, F., Merlet, B., Gloaguen, Y., et al. 2018. MetExploreViz: web component for interactive metabolic network visualization. Bioinformatics 34:312–3. doi: 10.1093/bioinformatics/btx588
[3] ↑ Johansen, T., Hansen, H. S., Richelsen, B., and Malmlof, R. 2001. The obese Gottingen minipig as a model of the metabolic syndrome: dietary effects on obesity, insulin sensitivity, and growth hormone profile. Comparat. Med. 51:150–5.
[4] ↑ https://www.scq.ubc.ca/a-brief-overview-of-metabolomics-what-it-means-how-it-is-measured-and-its-utilization/
