Abstract
Allergy is a syndrome characterized by an undesirable bodily reaction against a harmless substance. Allergies are very common, and the prevalence of allergic diseases has continued to grow over the last 50 years. It is not completely clear why some people develop allergic reactions and others do not. In this article, we explore how an allergic reaction occurs, as well as discuss the causes of allergy and its treatments.
Importance to Children and Teens
Allergy is a worldwide problem, and there is a high prevalence of allergic syndromes like allergic asthma and food allergies among children. It is important to understand what triggers and how to prevent/treat an allergic reaction. Not only that but highlight the usage of immunotherapy for allergic disorders and how they can improve the quality of life of non-drugs responders.
What Is an Allergy?
We all have a recognition and defense system in our bodies, which is called the immune system. The immune system is made up of cells, substances called antibodies, and many other components. When we are vaccinated or when we get infected by a microorganism that can cause disease, our immune system aims to develop cells and antibodies that will protect us against that specific microorganism. Antibodies are molecules produced by cells called B cells, and antibodies have the ability to bind to the invading microorganism, to prevent or combat an infection. However, in an allergy, the immune system reacts in a different way.
An allergy occurs when, for some reason, the immune system creates a response against a harmless substance, like pollen or a certain kind of food. Allergies are very common, and it is estimated that around one in three people has some type of allergy. Allergy can generate a reaction in any part of the body. For example, a food allergy can cause problems in the intestines, with symptoms, such as abdominal pain and diarrhea. Allergy can show up in the lungs in the form of allergic asthma, causing difficulty breathing and overproduction of mucus.
How Does an Allergic Response Happen?
When the body of an allergic person encounters an allergen (the substance that causes the allergic reaction), the immune system produces cells and antibodies against that harmless substance. Common allergens are shown in Figure 1. Some of the cells produced in an allergic response are called type 2 T helper cells (Th2), and these Th2 cells help other cells, called B cells, to produce a certain type of antibody called immunoglobulin E (IgE). The IgE then binds to other immune cells, making those cells very sensitive to the allergen. When the person comes into contact with that same allergen again, the immune cells coated with IgE release chemicals that cause inflammation and swelling, and those chemicals are the cause of the itching and sneezing symptoms that often occur in the body’s attempt to remove the allergen. The Th2 cells can also go to the site where the allergen entered the body and promote inflammation in that site. For example, the eyes of an allergic person can become swollen, red, and itchy in response to an allergen in the air, like pollen.
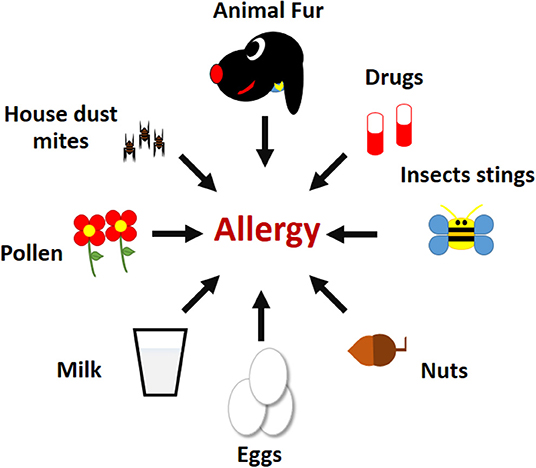
- Figure 1 - Examples of common allergens.
- Mites present in house dust, fur from domestic animals, compounds in drugs, venom and other substances presents in insect stings, nuts, eggs, milk, and pollen from flowers.
Why Do Only Some People Have Allergies?
Although we know a lot about how allergic reactions occur, the exact reason why some people develop allergies while others do not is still a mystery. We know that there is a genetic predisposition, meaning that if your mother or father have allergies, you are more likely to also have allergies. Factors in the environment also play a role in the likelihood of developing allergies [1–3], such as:
- Where you live (if it is rural or urban);
- Lifestyle factors (whether you exercise, for example);
- Dietary habits (the food you eat); and
- Medicines (antibiotics for example).
How Are Allergies Diagnosed?
To be sure that a person is allergic to something, a medical doctor can perform some simple tests. The most popular ones are called the skin-prick test and the IgE test.
In the skin-prick test, the doctor or nurse puts tiny amounts of different allergens just under your skin. If you are allergic, you will develop a red bump where the allergen was placed. The doctor can tell how allergic you are by the size of the red bump. In the IgE test, the doctor will do some blood tests to see whether you have a high amount of IgE in your bloodstream, or IgE specific to some common allergens.
How Are Allergies Treated?
If you have a positive allergy test, and you know which allergen(s) you are allergic to, the best treatment is to avoid contact with those allergens. However, it is easier to avoid contact with some allergens, like peanuts or milk, than it is to avoid airborne allergens, like dust or pollen. Can you imagine not being exposed to any pollen during spring? Since it is very hard to avoid some allergens completely, particularly the airborne ones, medicines have been developed to reduce inflammation and stop the allergic reaction from occurring.
If an allergic person is exposed to a very large amount of allergen, or if the person has a very severe allergy, that person may develop a serious, body-wide reaction that can be life-threatening. This reaction is called anaphylactic shock. Anaphylactic shock can occur very quickly after exposure to the allergen. The person’s blood pressure drops, he or she can have extreme difficulty breathing, and death can even result. Therefore, if you see someone having an anaphylactic shock, quickly call for help, because this is a true medical emergency.
Is There a Cure for Allergy?
The medicines developed to treat allergies are safe and helpful for relieving allergy symptoms, but they do not cure allergies [4]. For more than 100 years, scientists have been working on developing a cure for allergic disorders [5]. This is especially important because a part of the allergic population does not respond well to regular allergy medicines.
Currently, the only treatment with the potential for cure is called immunotherapy. Immunotherapy is a treatment that regulates a person’s immune system so that the person responds differently to an allergen. Immunotherapy is used for other diseases in addition to allergy, including as a treatment for certain types of cancer.
Immunotherapy for allergies involves giving increasing doses of the allergen to the allergic person, over time. There are two different allergy immunotherapies: subcutaneous, when the allergen is put under the skin of the patient (also called allergy shots) and sublingual, when the allergen is put under the tongue of the patient (also called allergy tablets). Both types of immunotherapy have strong and weak points, but they are both effective, to some extent, in reducing allergic reactions.
In general, allergy immunotherapy aims to teach the immune system to act differently, producing another kind of T cells, called T regulatory cells (Treg), and other types of antibodies, the blocking immunoglobulin G (IgG) (Figure 2). Treg cells encounter the Th2 cells and prevent their activation. IgG antibodies encounter the allergen before the allergen meets the IgE antibodies on immune cells, and this can help prevent the allergic reaction.
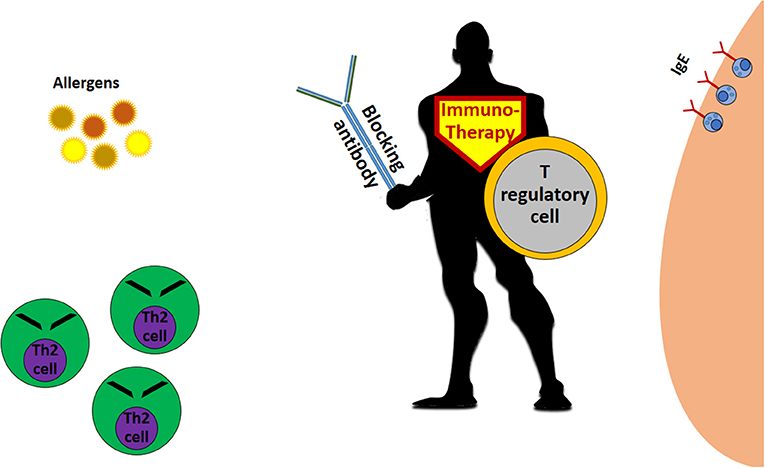
- Figure 2 - The allergy immunotherapy “superhero.”
- Immunotherapy for allergy works mainly through the creation of T regulatory cells, which inhibit allergy-causing Th2 cells and stimulate the production of blocking antibodies that prevent the allergen from coming in contact with the “allergy antibody,” IgE.
Summary
In conclusion, allergies are a serious health problem. Although there are medicines that relieve allergy symptoms, the only cure for allergy is the use of immunotherapy, which changes the patient’s response to the allergen. Immunotherapy is usually prescribed for patients that do not respond to the usual medicines. Scientists all over the world are still working on understanding allergies so that they can develop better treatments and possibly even a cure for allergies.
Glossary
Immunotherapy: ↑ Is a type of treatment that aims to modify how your immune system reacts to something, in the case of allergy immunotherapy it aims to modify the reaction to the allergen.
Allergen: ↑ Is normally a harmless substance, which in the case of an allergic person can trigger a response for the immune system and results in an allergic reaction.
Antibody: ↑ A Y-shaped protein produced B cells. Antibodies bind to microorganisms that infect the body, to neutralize them, and also to allergens, which creates an allergic response.
IgE: ↑ A type of antibody produced by an allergic person. IgE binds to certain cells of the immune system and causes an immediate allergic reaction if the person comes in contact with the allergen again.
Anaphylactic Shock: ↑ It is a severe, potentially life-threatening, allergic reaction. Some common symptoms include swelling of throat or tongue, difficulty breathing, vomiting, dizziness, and drop blood pressure.
IgG: ↑ A type of antibody that can be produced after allergy immunotherapy. IgG can prevent the immediate allergic reaction by binding to the allergen and blocking it, before the allergen binds to the IgE.
Conflict of Interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
References
[1] ↑ Alberca-Custódio, R. W., Greiffo, F. R., MacKenzie, B., Oliveira-Junior, M. C., Andrade-Sousa, A. S., Graudenz, G. S., et al. 2016. Aerobic exercise reduces asthma phenotype by modulation of the leukotriene pathway. Front. Immunol. 7:237. doi: 10.3389/fimmu.2016.00237
[2] ↑ Schröder, P. C., Li, J., Wong, G. W., and Schaub, B. 2015. The rural-urban enigma of allergy: what can we learn from studies around the world? Pediatr. Allergy Immunol. 26:95–102. doi: 10.1111/pai.12341
[3] ↑ Yilmaz, B., Carvalho, J. C., and Marialva, M. 2019. The intestinal universe—full of gut heroes who need sidekicks. Front. Young Minds 7:111. doi: 10.3389/frym.2019.00111
[4] ↑ Larsen, J. N., Broge, L., and Jacobi, H. 2016. Allergy immunotherapy: the future of allergy treatment. Drug Discov. Today 21:26–37. doi: 10.1016/j.drudis.2015.07.010
[5] ↑ Ring, J., and Gutermuth, J. 2011. 100 years of hyposensitization: history of allergen-specific immunotherapy (ASIT). Allergy 66:713–24. doi: 10.1111/j.1398-9995.2010.02541.x
