Abstract
Poor mouth care and heart disease are two major health concerns worldwide. Both conditions occur in humans and in many mammals, including our pets. “Periodontal” is the word used to refer to structures surrounding the teeth, including the gums and bone. Scientists have seen a connection between poor periodontal health and the increased risk of developing heart disease. It is thought that the bacteria found in dental plaque enters the bloodstream once the gums become inflamed. These bacteria travel through blood vessels, helping blockages called atherosclerotic lesions to form, which narrow the passageways of blood to the heart. In severe cases, lesions can dislodge from the arteries and completely block blood flow to the heart, leading to heart disease and heart failure. Scientific studies have shown that poor periodontal health significantly increases the risk of developing heart disease. Interestingly, it seems our canine companions are suffering the same effects. Brushing teeth could save lives!
What Are Periodontal Disease and Heart Disease?
Periodontal disease happens when structures surrounding the teeth, including the gums and bone get infected by bacteria. You might think that periodontal disease only affects the mouth, but around a century ago, scientists suggested a theory that periodontal disease may cause problems in vital organs, particularly the heart. In more recent years, several scientific studies have directly investigated the link between periodontal disease and coronary heart disease (also called cardiovascular disease). Coronary heart disease is caused when blood vessels to the heart become narrow or blocked, it is common in people and can be a very serious problem. Although several factors have been linked to heart disease, including smoking, limited access to healthcare, poor diet, drinking too much alcohol and lack of exercise, periodontal disease also plays an important part. Links between poor periodontal health and an increased risk of heart disease (especially a heart infection called endocarditis) and lung disease have been discovered. Research in America showed that 70% of adults over 65 years old and 47% of adults over the age of 30 have some periodontal disease [1]. Heart disease causes around 1 out of every 4 deaths, and animals suffer from heart disease that is very similar to ours (see Frontiers Young Minds article “Mending a Broken Heart” [2, 3]). Studies on dogs have also questioned whether dogs with poor periodontal health also have increased risks of developing health issues, such as cardiovascular disease.
How Is Periodontal Disease Related to Heart Disease?
While studies have shown links between periodontal and heart disease in humans and dogs, exactly how one leads disease to the other needs further investigation. Researchers have proposed that bacteremia (bacteria in the bloodstream) is the main cause. There are more than 700 species of bacteria that can live in the mouth, and some of these bacteria can move from the mouth into the blood [4]. The tongue, palate, cheeks, and teeth each have their own diverse range of bacteria. Due to the high numbers and variety of bacteria in the mouth, bacteremia occurs naturally as a result of tooth brushing and chewing. Normally, these bacteria are cleared from the blood by the immune system and no infection develops. However, in people with severe periodontal disease, the gums (also called gingiva) become inflamed, resulting in a condition called gingivitis. Gingivitis can often be treated with good mouth care and help from dentists, but the inflammation can enable oral bacteria to be released directly into the bloodstream (Figure 1), increasing the risk of bacteremia. The bacteria travel through blood vessels contributing to the creation of plaque-like structures that stick to, and narrow, blood vessel walls. This is known as atherosclerosis, and it can reduce blood flow to the heart (Figure 2).
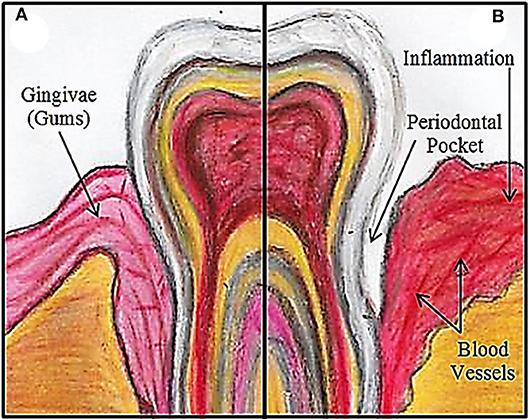
- Figure 1 - (A) A healthy tooth/gum.
- The gums (gingiva) are a pink color, with no gaps (periodontal pockets) between the tooth and the surrounding gum. (B) Changes that occur in periodontal disease. The gingiva becomes reddened due to increased blood vessels, and inflammation develops. These changes create a way for bacteria to directly enter the bloodstream. Periodontal pockets form if plaque builds up on teeth over a long time. Plaque build-up causes bacteria to develop and destroy the surrounding gum, pulling it away from the tooth’s surface. The pockets deepen over time, as more plaque develops.
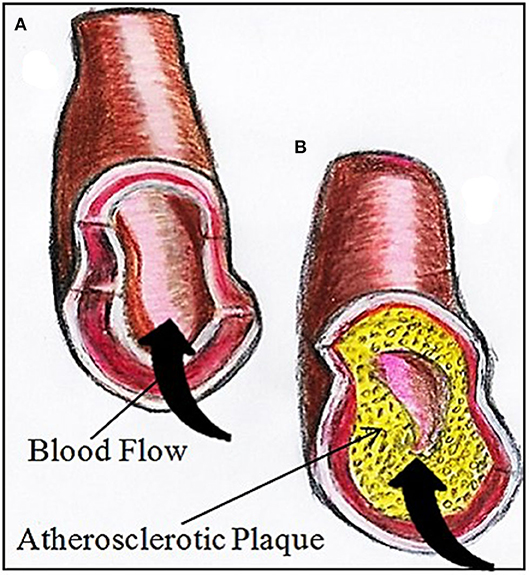
- Figure 2 - (A) A normal artery should have smooth and wide inner walls, allowing the blood to flow freely with no restrictions.
- (B) An artery with atherosclerosis has plaque build-up narrowing the inside of the artery, making the walls bumpy. Blood flow is restricted, meaning that less blood can be delivered to vital organs, such as the heart and brain, increasing the risk of heart attacks and strokes.
Sometimes the plaques can rupture, creating a clot that can circulate around the body. Clots can become lodged in vital organs, such as the heart or brain, blocking blood supply completely. In some cases, bacteria travel to the heart and stick to heart valves and other parts of the heart. If this is not treated quickly, a condition known as endocarditis can develop (Figure 3). Endocarditis can damage or destroy the heart valves, leading to life-threatening complications. Studies show that poor periodontal health in humans doubles the chance of developing heart disease, compared to people with healthy gums.
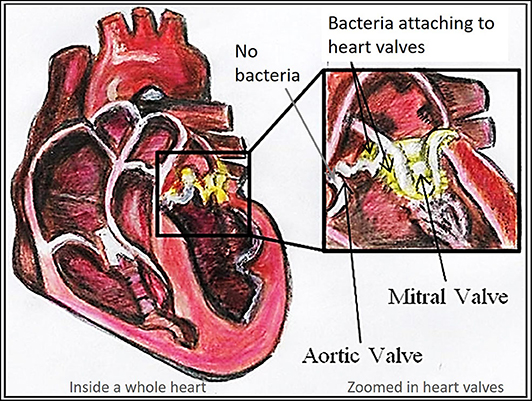
- Figure 3 - Bacterial endocarditis infecting two heart valves.
- Most of the bacteria have attached to the mitral valve and there is some build-up of bacteria on the right-hand side of the aortic valve. Bacteria are shown in yellow. The left-hand side shows what a normal valve (with no bacteria, shown by a gray arrow) should look like.
In people, certain dental and medical procedures can also cause an overload of bacteria in the bloodstream; this can result in bacteremia if a person is already unwell or has a weakened immune system. Therefore, people suffering from heart disease or damaged heart valves sometimes take antibiotics before dental procedures. Antibiotics help destroy bacteria or control their numbers in the body and help prevent bacterial endocarditis from developing. However, because antibiotic resistance (when antibiotics are no longer able to kill bacteria because the bacteria have become resistant to them) is becoming a big concern worldwide, it is important that antibiotics are only used when necessary—another reason to keep your teeth and gums healthy!
Research has also found that people with diabetes, especially if it is uncontrolled, have an increased risk of developing periodontal disease. People with diabetes have high levels of sugar in their blood, because they cannot break it down properly. High blood sugar levels cause bacteria to multiply more rapidly, meaning more bacteria can enter the bloodstream and cause bacteremia.
Periodontal disease is not just isolated to the mouth; it causes inflammatory reactions throughout the whole body. Consequently, periodontal disease can make diabetes more severe, because one of the factors contributing to diabetes is chronic inflammation. The British Heart Foundation reported that people with moderate to severe periodontal disease had a 69% increased risk of developing diabetes [5].
What About the Oral Health of Our Pets?
Until recently, the effects of poor periodontal health on the rest of the body had not been investigated in dogs. This is surprising, because periodontal disease is a very common problem in dogs today, especially in small-breed dogs. Almost every domestic dog and cat (75%) will develop some type of periodontal disease by the time they reach 4 years old [6].
One scientist conducted a study examining the veterinary records of 60,000 dogs with periodontal disease and 60,000 without it [7], and demonstrated a link between periodontal disease and heart disease. As with people, there are multiple possible causes of heart disease in dogs, but improving dental care is essential. Dogs can die from heart problems, even at a young ages.
So, How Do I Keep My Teeth Healthy?
As with most things in life, prevention is better than cure. Did you know that toothpastes were initially made from harsh, gritty substances like chalk and jeweller’s polish? Along with removing nasty stains, they also wore away people’s teeth! In the nineteenth century, people mixed salt and sugar with water to make a paste, because they did not realize sugar was bad for their teeth. It is probably better to stick to the tips below to maintain a healthy mouth.
Humans spend 38.5 days of their lives cleaning their teeth, however, plaque can start to form just 4 h after brushing. It is important to brush your teeth for at least 2 min, twice a day. The best time to brush teeth is before bed at night. Brushing teeth also provides the perfect opportunity to look for warning signs of gum disease, which include red or swollen gums, bleeding during or after brushing, and persistent bad breath. If you are worried about any of these symptoms, it is important to tell your dentist.
Fluoride works by hardening tooth enamel and reducing the risk of developing tooth decay, so make sure your toothpaste has fluoride in it. For the past 70 years, fluoride has also been added to drinking water to improve dental health. It was first introduced in the United States in 1945, and in Britain, fluoride was first added in Birmingham in 1964. The level of fluoride in drinking water is now 1 mg per liter of water, the appropriate level to reduce tooth decay.
Diet also plays an important role in protecting your teeth. Limiting your intake of acidic soft drinks and fruit juices can prevent the softening of enamel, which can lead to cavities forming. Your saliva acts to stabilize the pH of your mouth, providing a stable environment for tooth enamel. Drinking plenty of water helps your saliva to work most effectively. Research has also shown that mouthwash is good for oral hygiene.
How Do I Keep My Dog’s Teeth Healthy?
Brushing your dog’s teeth daily with a specially designed toothbrush and toothpaste that is made for dogs (fluoride in human toothpaste can be toxic to dogs) will help their teeth and gums. Giving your dog dental chews 2–3 times weekly will reduce plaque accumulation. Since these treats can be high in calories, reduce your dog’s food intake accordingly. You can also take your pet to the vet for regular dental and general health check-ups.
The Future of Periodontal and Heart Health
Since the connection between oral disease and heart disease is present in humans and in dogs, it would be useful to use dogs to identify whether certain genes are responsible for linking periodontal and heart disease. Finding the responsible genes will help scientists to understand how the two diseases are related. We are also finding that poor periodontal health can affect other vital organs, such as the kidneys and liver, too. In conclusion, it is important to make good daily oral hygiene a top priority, from a young age. A healthy mouth will help your periodontal and heart health and may have other health benefits as well. Keep brushing, flossing, and seeing your dentist!
Glossary
Periodontal Disease: ↑ Infection of the structures surrounding the teeth, including the gums, ligaments, and bones.
Coronary Heart Disease: ↑ A common problem caused by blood vessels to the heart becoming narrow or blocked, this reduces blood flow to the heart.
Endocarditis: ↑ An infection of the inner lining of the heart chambers and valves (known as the endocardium).
Bacteremia: ↑ A condition caused by the entry of bacteria into the bloodstream through the mucous membranes or skin.
Gingiva: ↑ The medical word used to describe the gums in the mouth which surround the teeth and lining the mouth.
Gingivitis: ↑ Inflammation of the gums, which is reversible. Gingivitis usually occurs before periodontitis (gum disease), which is irreversible.
Atherosclerosis: ↑ A condition caused by a build-up of fatty material (called a plaque or lesion) in and on artery walls. This can narrow blood vessels, restricting blood flow to the heart.
Conflict of Interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
Acknowledgments
The authors would like to thank our informal young reviewers; Hannah Clark, Holly-Marie Broadhurst, Rebekah Kippax, Taylor Lewys Davies, and Harry Saunders. Part of this work was made possible due to INSPIRE student scholarships funded by The Wellcome Trust, The Academy of Medical Sciences. This grant awarded to Drs. V. James, N. Mongan, J. Daly, C. S. Rutland, K. Braithwaite, P. Voigt, and K. Cobb to promote research and public engagement. We would also like to thank the British Science Association and University of Nottingham for awarding CR with a BSA Media Fellowship 2019. We also thank the Anatomical Society for helping to fund this work a Public Engagement and Outreach grant to CR titled Anatomy for ALL—Making Anatomy Accessible.
References
[1] ↑ Eke, P. I., Dye, B. A., Wei, L., Thornton-Evans, G. O., Genco, R. J., and CDC Periodontal Disease Surveillance. 2012. Prevalence of periodontitis in adults in the United States: 2009 and 2010. J. Dent. Res. 91:914–20. doi: 10.1177/0022034512457373
[2] ↑ Simpson, S., Rutland, P., and Rutland, C. S. 2017. Genomic insights into cardiomyopathies: a comparative cross-species review. Vet. Sci. 4:19. doi: 10.3390/vetsci4010019
[3] ↑ Clark, N., Alibhai, A., and Rutland, C. S. 2018. Mending a broken heart—the genetics of heart disease. Front. Young Minds 6:19. doi: 10.3389/frym.2018.00019
[4] ↑ Aas, J. A., Paster, B. J., Stokes, L. N., Olsen, I., and Dewhirst, F. E. 2005. Defining the normal bacterial flora of the oral cavity. J. Clin. Microbiol. 43:5721–32. doi: 10.1128/Jcm.43.11.5721-5732.2005
[5] ↑ Preshaw, P. M., Alba, A. L., Herrera, D., Jepsen, S., Konstantinidis, A., Makrilakis, K., et al. 2012. Periodontitis and diabetes: a two-way relationship. Diabetologia 55:21–31. doi: 10.1007/s00125-011-2342-y
[6] ↑ Carinci, F., Martinelli, M., Contaldo, M., Santoro, R., Pezzetti, F., Lauritano, D., et al. 2018. Focus on periodontal disease and development of endocarditis. J. Biol. Reg. Homeos. Ag. 32:143–7.
[7] ↑ Glickman, L. T., Glickman, N. W., Moore, G. E., Goldstein, G. S., and Lewis, H. B. 2009. Evaluation of the risk of endocarditis and other cardiovascular events on the basis of the severity of periodontal disease in dogs. J. Am. Vet. Med. A 234:486–94. doi: 10.2460/javma.234.4.486
