Abstract
Amyotrophic lateral sclerosis (ALS) is a serious disease of the nervous system, in which the brain and spinal cord cannot communicate properly with the muscles to coordinate the body’s movements. Consequently, the muscles gradually stop working and things like walking, eating, breathing, and speaking become more and more difficult. Many aspects of ALS remain a mystery, but we know that cells called neurons run out of energy in ALS patients, resulting in the loss of communication with muscles. This happens due to defects in mitochondria—the tiny structures within our cells that produce energy. Researchers have been working hard to discover how to keep mitochondria healthy, avoid the death of nerve cells, and ultimately restore the communication between neurons and muscles.
What Is Amyotrophic Lateral Sclerosis?
The brain and spinal cord control every little thing we do, such as thinking, moving, feeling, and learning. They even control things we are not aware of, such as heartbeat, breathing, and digestion. But they cannot do everything alone! The brain and spinal cord are connected to each organ and muscle by cells called neurons (Figure 1A).
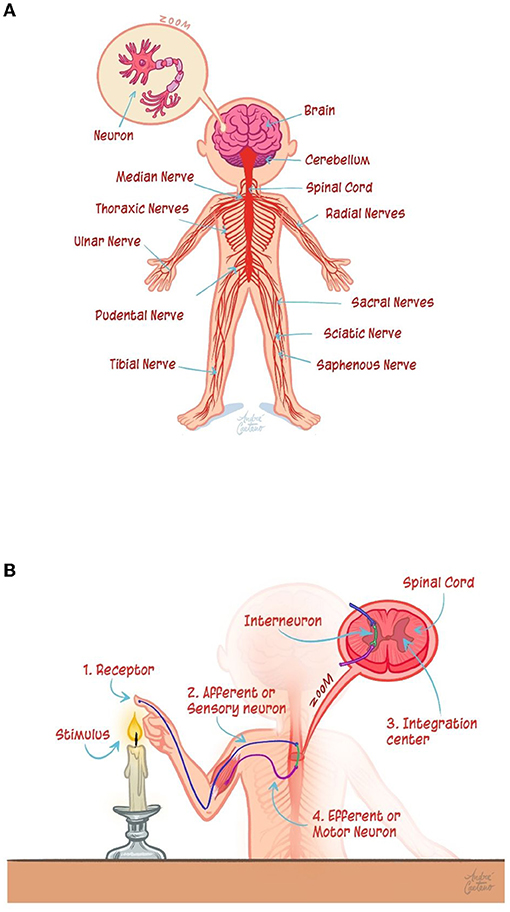
- Figure 1 - (A) The brain and spinal cord control the body with the help of neurons, which make up the many nerves that connect to all the body’s organs.
- (B) When you touch something hot, the sensory neurons in your skin send a message of pain to the spinal cord. As a result, through the motor neurons, the spinal cord immediately tells the muscles of the arm to contract, removing your hand from the heat. When this precise coordination is not working properly, as happens in ALS, the malfunctioning motor neurons may be unable to send information to the muscles, and the muscles gradually stop working.
The human body contains billions of neurons, which work every second of our lives. Neurons communicate with each other inside the brain, and they also communicate with the various parts of the body, controlling all body functions. For example, when you touch a hot surface, the heat sensors in your skin communicate with neurons that send a message of pain to your spinal cord, which immediately returns a message back to contract the muscles in your arm so that you pull away (Figure 1B). The neurons responsible for muscle contraction are called motor neurons, and they control every movement of the body.
In neurodegenerative diseases, some neurons do not work properly. This is what happens in amyotrophic lateral sclerosis (ALS), a disease in which the motor neurons get sick and can no longer effectively communicate with the muscles. Consequently, the muscles in the entire body gradually stop working. Because ALS evolves rapidly, within a few months ALS patients develop difficulties walking, eating, breathing, and speaking (Figure 2). Thus, ALS is a devastating disease and patients need a lot of support, both from other people and from mechanical devices like wheelchairs. ALS is generally diagnosed in people aged 54–69, and it affects 4–8 people out of 100,000 [1].
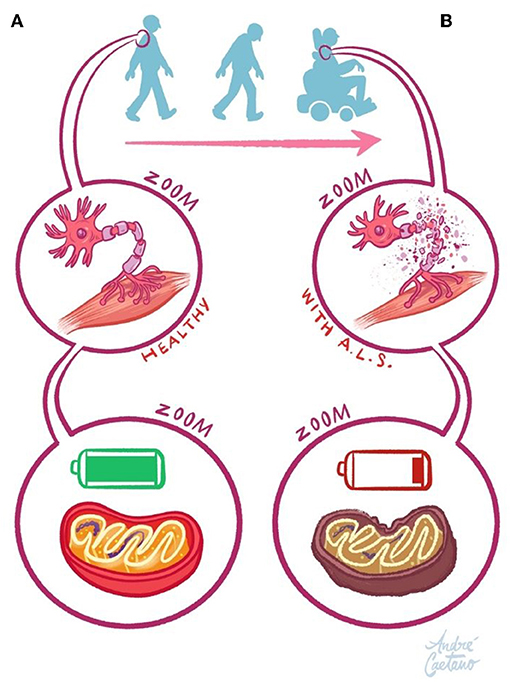
- Figure 2 - (A) Like all cells, neurons need energy to work properly.
- This energy is provided by the mitochondria—the cells’ batteries. Since neurons are constantly working, they rely on a precise and continuous supply of energy. As such, neurons contain numerous mitochondria. (B) However, if something interferes with the function of mitochondria, energy production is affected and neurons “run out of power.” When this happens, the communication between motor neurons and muscle cells fails, resulting in ALS.
Why Do Neurons Fail to Communicate With Muscles?
Just like every cell of the body, neurons need energy to work. Think of neurons as your mobile phone—if your phone runs out of power, you can no longer communicate with your friends. That is what happens to the motor neurons of ALS patients—they run out of energy and become unable to communicate with their respective muscles (Figure 2).
The power needed by neurons (and all other cells) comes from cell parts called mitochondria, which function as cellular batteries. Different types of cells contain different numbers of mitochondria, depending on how much energy they need—the more energy a cell needs, the more mitochondria it will have. Since neurons are constantly working, they have a lot of mitochondria. Did you know that the brain consumes 20% of the body’s energy? Because neurons need so much energy to perform their important functions, small defects in energy production can lead to neuron death, which can cause the development of neurodegenerative diseases. Beyond decreased energy production, studies in ALS patients discovered that the mitochondria of their motor neurons may have other problems, too [2].
What Is Oxidative Stress?
Oxidation is a natural process that happens when something is in contact with oxygen, such as when you cut an apple and leave it in contact with the air for hours (Figure 3A). Something similar occurs inside our cells when cellular components are in contact with reactive oxygen species (ROS). ROS are molecules that steal electrons from other molecules. In normal conditions, ROS are important for controlling critical cellular processes. But when excessive amounts of ROS are produced and our cells cannot cope with them, ROS start to damage essential cellular components, including mitochondria. This is called oxidative stress, and it can kill cells (Figures 3B, C).
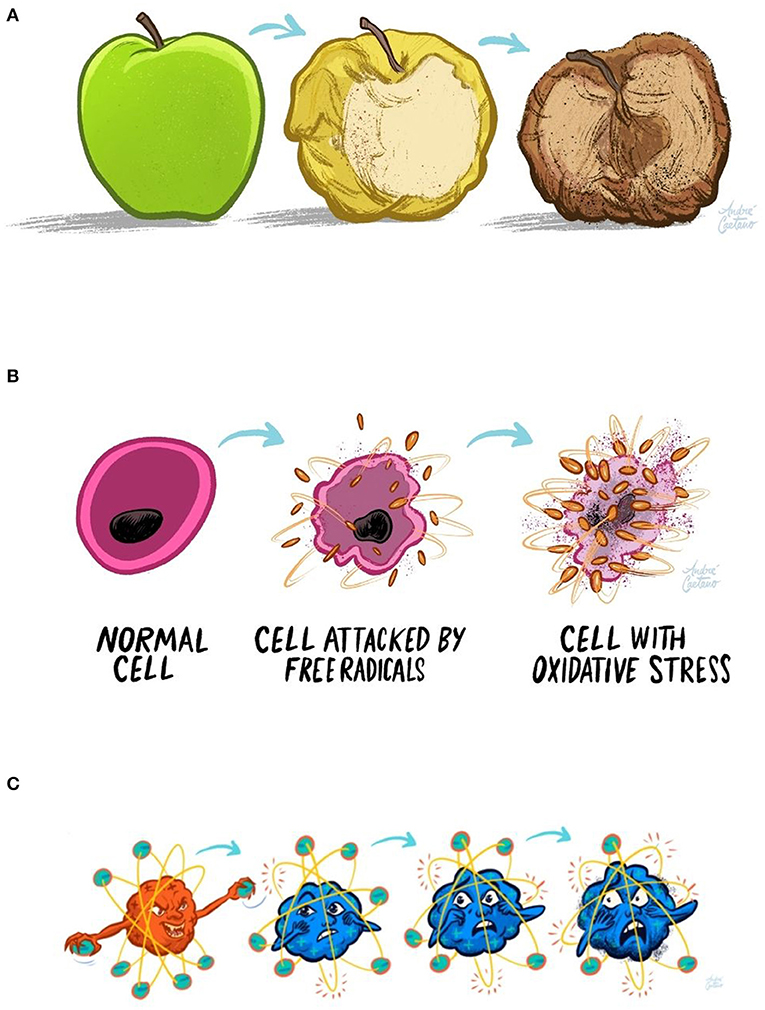
- Figure 3 - (A) If you cut an apple and leave it in the air, the oxygen causes it to turn yellow and shriveled, and it eventually becomes brown and dried.
- This process is called oxidation. (B, C) A similar process occurs when the inner components of our cells interact with reactive oxygen species (ROS) or free radicals, molecules that try to steal electrons from other molecules. If the cell cannot neutralize ROS, a condition called oxidative stress results, which can cause cell damage and even death. This is believed to be how the loss of motor neurons occurs in ALS.
When mitochondria are not working properly, neurons become more susceptible to damage from oxidative stress, and the neurons can no longer perform their functions. High levels of oxidative stress in the motor neurons of ALS patients lead to mitochondrial damage that prevents neurons from communicating with muscles [2, 3].
What Causes ALS and How Can We Treat It?
The brain and neurons are extremely complex, and we still do not know exactly what causes ALS or how to treat it. We know that 10% of ALS patients inherit the disease from their parents (called familial ALS), while in the remaining 90% of cases there is no clear origin (called sporadic ALS) [4]. Both familial and sporadic ALS are associated with mutations in more than 50 genes [5]. Certain behaviors, including smoking, being overweight, lack of physical activity, and exposure to pesticides or heavy metals, have been identified as risk factors for ALS—but we still do not understand the exact role of these factors in causing the disease [6].
ALS remains incurable and the therapies that are available only help with symptoms [7]. But scientists have been exploring possible treatment ideas, including the use of substances called antioxidants, which can decrease ROS levels and reduce oxidative stress in motor neurons. These antioxidants may keep mitochondria healthy, keep motor neurons alive, and restore communication between motor neurons and muscles. Researchers worldwide are seeking to unravel the mechanisms behind ALS to better understand how this disease progresses. This knowledge could lead to the identification of biomarkers (indicators of the disease that can be measured, for example, molecules that could be detected by blood tests) that would allow us to diagnose ALS earlier. Research could also help us develop potential drugs to treat the disease. As each case of ALS has its own characteristics, it might be necessary to customize treatments for each individual. Until we have a successful treatment for ALS, we will continue to work hard to discover ways to help ALS patients and their families.
Glossary
Neurons: ↑ Cells of the nervous system that communicate with each other and link the brain and spinal cord to all organs in the body. Motor neurons control movement.
Neurodegenerative Diseases: ↑ Diseases caused by the loss of structure or function of neurons that affect many of your body’s activities—balance, movement, talking, breathing and heart function, for example.
Mitochondria: ↑ Cellular components responsible for energy production.
Oxidation: ↑ Reaction of an element with oxygen.
Reactive Oxygen Species (ROS): ↑ Highly reactive molecules produced by cells that steal electrons from other molecules, damaging them.
Oxidative Stress: ↑ Imbalance between ROS and antioxidants in the body, which can lead to cell damage.
Antioxidants: ↑ Molecules that decrease oxidative stress by donating electrons to other molecules.
Biomarker: ↑ Biological indicator of a biological state.
Acknowledgments
We are grateful to André Caetano for the illustrations included in this article. This work was financed by the European Regional Development Fund (ERDF), through the Centro 2020 Regional Operational Programme (POCI-01-0145-FEDER-029391, POCI-01-0145-FEDER-028607); by COMPETE 2020–Operational Programme for Competitiveness and Internationalization, under the project CENTRO-01-0145-FEDER-000012 Healthy Aging 2020; by Portuguese funds via FCT–Fundação para a Ciência e a Tecnologia (POCI-01-0145-FEDER-029391, PTDC/MED-FAR/29391/2017, UIDB/04539/2020, UIDP/04539/2020, LA/P/0058/2020); by European Social Fund (Post-Doctoral Researcher contract DL57/2016 #SFRH/BPD/84473/2012 to AD).
Conflict of Interest
FS was employed by Mitotag, Biocant Park, Parque Tecnológico de Cantanhede.
The remaining authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
References
[1] ↑ Longinetti, E., and Fang, F. 2019. Epidemiology of amyotrophic lateral sclerosis: an update of recent literature. Curr. Opin. Neurol. 32:771–6. doi: 10.1097/WCO.0000000000000730
[2] ↑ Cunha-Oliveira, T., Montezinho, L., Mendes, C., Firuzi, O., Saso, L., Oliveira, P. J., et al. 2020. Oxidative stress in amyotrophic lateral sclerosis: pathophysiology and opportunities for pharmacological intervention. Oxid. Med. Cell Longev. 15:5021694. doi: 10.1155/2020/5021694
[3] ↑ Carrera-Juliá, S., Moreno, M. L., Barrios, C., de la Rubia Orti, J. E., and Drehmer E. 2002. Antioxidant alternatives in the treatment of amyotrophic lateral sclerosis: a comprehensive review. Front. Physiol. 11:63. doi: 10.3389/fphys.2020.00063
[4] ↑ Smith, E. F., Shaw, P. J., and De Vos, K. J. 2019. The role of mitochondria in amyotrophic lateral sclerosis. Neurosci. Lett. 710:132933. doi: 10.1016/j.neulet.2017.06.052
[5] ↑ Boylan, K. 2015. Familial ALS. Neurol. Clin. 33:807–30. doi: 10.1016/j.ncl.2015.07.001
[6] ↑ Nowicka, N., Juranek, J., Juranek, J. K., and Wojtkiewicz J. 2019. Risk factors and emerging therapies in amyotrophic lateral sclerosis. Int. J. Mol. Sci. 20:2616. doi: 10.3390/ijms20112616
[7] ↑ Ramalho-Santos, J., Quatorze, M., and Amaral, S. V. 2020. Journey around A.L.S. Center for Neuroscience and Cell Biology. Available online at: https://cnc.uc.pt/en/resources (accessed April 28, 2023).
