Abstract
Sometimes in life, we can get sick and feel badly—maybe a headache, fever, or other uncomfortable symptoms—and sometimes we need to use a medicine to feel better. Medicines can often taste sweet, have bright colors, or even look like candy. But be careful, medicines are certainly not candy! They are powerful substances capable of curing, treating, and preventing diseases. If we do not use medicines properly, they can be very dangerous or even kill us. That is why it is important to keep medicines in safe places, away from children and animals, and use them only under adult supervision. The best way to practice medicine safety is to learn as much as possible about our medicines and follow the recommendations of our healthcare professionals.
Most everyone has been sick or at least knows someone who was sick and had to take a medicine to get better. But what are medicines, and when are they needed? Although we usually think of medicines as substances used to treat or cure diseases, they can also be used for other purposes. Some medicines can prevent us from getting sick at all, some relieve the symptoms of diseases we already have, and others control the development of diseases that have no cures. Medicines are produced by scientists who work in pharmaceutical industry. These scientists work for many years to figure out how each drug works in the human body.
Did you know that, in 2021, ~1.4 billion dollars was spent on medicines all over the world? That is a lot of money! But there were also countless lives saved as well as diseases treated or prevented. Medicines come in many forms: tablets, capsules, syrups, ointments, creams, sprays, and more. All these medicines are the result of decades of studies designed to produce forms that are both safe and easy to use.
Why Are Some Medicines So Tasty?
Sometimes medicines have bright colors and a sweet taste. But be careful! Despite tasting like candy, you cannot just eat them any time you want. So why do pharmaceutical companies make medicines so tasty? Medicines are made up of two main components: active substances, which are the chemicals that actually help our bodies, and excipients, which are additional substances added into medicines to make them easier to use. Some active substances taste bad, so pharmaceutical companies add excipients into the recipe, to mask the bad taste and make the medicine easier to swallow. For example, they add sweeteners, which make medicines sweeter, and flavorings, which provide tasty flavors to the medicine, such as cherry. Despite sometimes tasting like candy, medicines should only be used according to the directions of the health professional who prescribed them.
Risks of Self-Medication
Although medicines help with our health, if we do not take them properly they can also harm us. Sometimes the instructions that come with medicines can be complicated and confusing, which makes it easy for mistakes to happen. Some people try to use medicines without a doctor’s recommendation. This is called self-medication, and it can be dangerous. Next, we will describe several of the risks of self-medication (Figure 1) [1, 2].
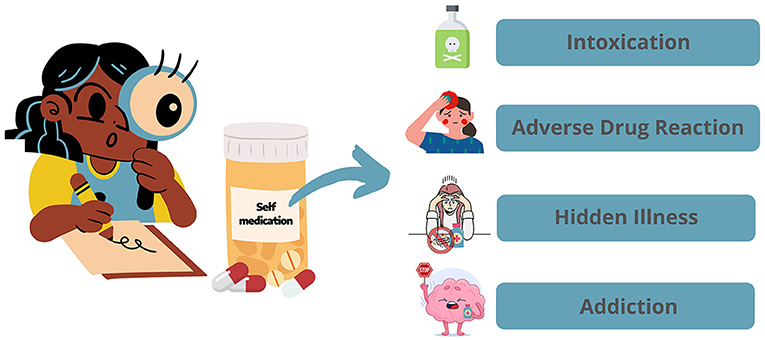
- Figure 1 - Self-medication, or take a medicine without health professional orientation, is dangerous and can have many risks.
- Medicines should never be taken without the recommendation of a doctor or other health professional.
Poisoning
Poisoning is the harm that can come to humans and animals after they contact certain chemicals. Some symptoms of poisoning include vomiting, difficulty breathing, skin sores, and skin redness. Poisoningcan also happen after taking too much of a medicine. Poisoning is serious—it causes thousands of deaths across the world. According to the World Health Organization, acute poisoning is associated with ~45,000 deaths per year among children and adolescents under 20 years of age [3].
No matter how harmless a medicine may appear, it can cause a lot of health damage. Each year, more than 38,000 children in Brazil alone go to the emergency room after taking medicines without adult supervision [4]. Can you imagine how many children that would equal the world over?
Adverse Drug Reactions
Adverse reactions, unlike poisoning, occur unintentionally, at doses considered safe. Harmful and unwanted effects that happen following the use of a medicine are called adverse drug reactions. They can be classified into two types: Type A and Type B.
Type A adverse reactions happen when too much medicine is used. These reactions are common, the symptoms are predictable, and they can occur in anyone who takes the medicine. An example is a person with diabetes who uses a medicine to lower their blood sugar. If they take too much of the medicine, their blood sugar will become too low, to the point that the person feels sick [5].
Type B adverse reactions are unexpected, which means that they may not have been discovered when the medicine was being tested. These are uncommon reactions and do not depend on the dose of medicine used. Type B reactions usually occur in people who have some type of allergy or other susceptibility [5]. For example, some vaccines are made from chicken eggs, so people who are allergic to eggs will have allergic reactions to these vaccines.
Hidden Illnesses
It is important to pay attention to the signals our bodies send us, because they may be the early symptoms of a disease. If we regularly self-medicate to relieve some symptom we are experiencing, we run the risk of masking the warning signals that our body is giving us, and we may not investigate the real cause of that symptom. This means we might fail to discover a developing disease that the body is trying to warn us about.
Addiction
We are used to thinking of addiction problems only in terms of illegal drugs, like cocaine or heroin. But did you know that medicines can also cause addiction? When medicines are misused—in excessive doses, for a longer period of time than necessary, or without the advice of a health professional, they can changes our bodies such that we need and want more and more of the medicine, even if it is not necessary to treat a disease. This is such an important problem that health professionals are taught to closely review a patient’s diagnosis, to make sure they need to use certain medicines [4]. Some stronger painkillers, such as morphine, can easily cause addiction.
Proper Storage of Medicines Is Important
When medicines are developed by pharmaceutical companies, several tests are done to make sure the medicines are safe and to determine the best storage conditions for each product. Ideal storage conditions must be maintained to ensure that medicines continue to work properly. Not every medicine has the same characteristics, so they should not all be stored in the same place. For example, some need to be stored at lower temperatures, like in the fridge, while others must remain at room temperature. Storage information can be found on the packaging or paper insert that comes with the medicine. In general, medicines should be stored in safe, ventilated, humidity-free places, protected from light and heat. They must be kept in their original packaging, so that they are easy to identify and the expiration date is known (Figure 2).
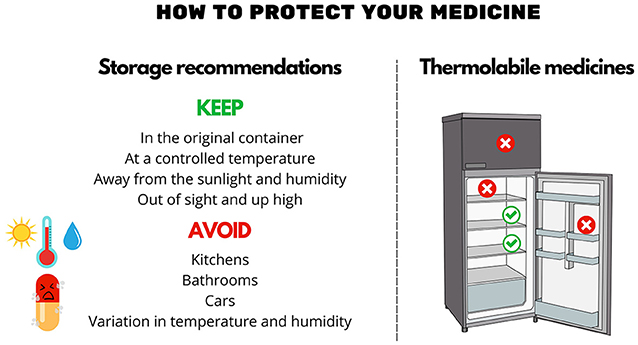
- Figure 2 - Each medicine needs to be stored under specific conditions so that it will not break down and will continue to work as it should.
- Be sure to read the storage conditions for all medicines. They can be found on the packaging or on the paper insert inside the box.
Avoid storing medicines in places that have a lot of temperature variation, such as above the fridge, in the kitchen, in the bathroom, or in the car. This helps to guarantee that the medicine will not break down and will keep working as intended.
Medicines that need to be kept in the fridge are known as thermolabile medicines. Some areas of the fridge have less temperature variation and are better for keeping medicines at the ideal temperature. The shelves in the middle of the fridge are best, while the doors and any shelves next to the freezer should be avoided.
It is very important to remember to keep medicines out of sight and high up, so that children and pets cannot reach them. This precaution can prevent accidental poisoning and ensure the safety of the whole family.
In conclusion, medicines are very important for our health, they help us to improve and prevent diseases. But we need to be very careful, because if used in the wrong way, they can lose their effect or cause us harm. To avoid this, we must always be guided by a health professional before taking any medication. And no matter how tasty the medicine is, never take more than recommended and always with adult supervision.
Glossary
Pharmaceutical Companies: ↑ Is responsible for developing drugs. From research to development and commercialization.
Active Substance: ↑ Is responsible for the effect of the drug.
Excipient: ↑ It is what pharmacists add to medicine to make it last longer and taste better.
Self-Medication: ↑ It is when a person takes the medicine without the guidance of a health professional. This practice can harm our health.
Adverse Drug Reactions: ↑ It is when we take a medicine, in a dose considered safe, but even so we have an unwanted effect. It occurs unintentionally and in few people.
Addiction: ↑ It is a dependence that a person has on something. In the case of medication, the patient, even without the need or illness, cannot stop taking the medication.
Thermolabile: ↑ When a product or substance loses its characteristics/safety with an increase in temperature. Medicines have a temperature range that can be stored.
Conflict of Interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
References
[1] ↑ Moraes, C. G., Mengue, S. S., Tavares, N. U., and Dal Pizzol, T. S. 2013. Utilização de medicamentos entre crianças de zero a seis anos: um estudo de base populacional no sul do Brasil [Drug use among children between zero and six years old: a population baseline study in the south of Brazil]. Cien Saude Colet. 18:3585–93. Portuguese. doi: 10.1590/s1413-81232013001200015
[2] ↑ Baskar, A., George, N., Sarika, M. L., and Ramamoorthy, L. 2020. Self-medication practices: a threat to health care. Indian J. Community Med. 45:388–9. doi: 10.4103/ijcm.IJCM_368_19
[3] ↑ Halhalli, H. C., and Uslu, T. 2021. Evaluation of pediatric patients admitted to the emergency department due to drug intoxication. Cureus. 13:e13366. doi: 10.7759/cureus.13366
[4] ↑ Melo, M. T. B., Santana, G. B. A., Rocha, M. H. A., Lima, R. K. S., Silva, T. A. B. D., Souza, C. D. F., et al. 2022. Epidemiological profile and temporal trend of exogenous intoxications in children and adolescents. Rev. Paul. Pediatr. 40:e2021004. doi: 10.1590/1984-0462/2022/40/2021004IN
[5] ↑ Edwards, I. R., and Aronson, J. K. 2000. Adverse drug reactions: definitions, diagnosis, and management. Lancet. 356:1255–9. doi: 10.1016/S0140-6736(00)02799-9
