Abstract
Of all people living on the planet today, there are an estimated 2 billion who do not have access to essential medicines and vaccines. Most of them live in developing countries. While scientific breakthroughs are leading to the development of new medicines to treat or cure many diseases, these fail to reach everyone who needs them. Even medicines that have been known for a long time are hard to get a hold of in certain parts of the world! This is called the access-to-medicine issue. In this article, we will explore four distinct approaches where pharmaceutical companies can improve their efforts on this issue, namely: availability, accessibility, affordability and acceptability.
What is the Access-to-Medicine Issue?
Accessing essential medicines and vaccines is critical for someone to be able to live free from disease. Sadly, there is an estimated 2 billion people on the planet who do not have access to these health products today, most of them living in developing countries. This situation is called the access-to-medicine issue, which stems from the “4As”: Availability, Accessibility, Affordability, and Acceptability. The lack of access to medicine is unfair and causes extensive amounts of pain and suffering. It can also push people into poverty. The companies that discover and manufacture medicines, called pharmaceutical companies, play an influential role in the access-to-medicine issue. Indeed, as they invent, produce, and supply most of the medicines in the world, these companies also have an important responsibility to help all people get access to medicines, through the 4As (Figure 1)1.
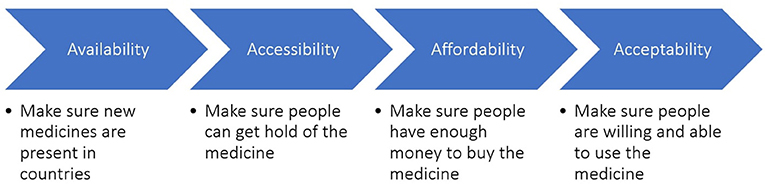
- Figure 1 - The 4As of access to medicine.
Availability
New medicines and other life-saving products must be made rapidly available to the people who need them, wherever they live. Most medicines are made by pharmaceutical companies in China, India, and the United States. However, regardless of where they are made, pharmaceutical companies should make sure that patients living in other countries have access to medicines. In order to do this, pharmaceutical companies need to register their products and ship them to countries where there is a need. If a medicine is not registered in a country, the product cannot be sold there. While this sounds like an easy procedure, less than one-quarter of recently launched medical products have been filed for registration in most countries that are in need of them [1].
The reason that many medicines are not registered is because customizing the registration to meet the strict requirements of every country can be a hard task for a company, especially since the criteria may vary from one country to another. Furthermore, the registration process can take a long time in some countries with poor healthcare systems. While registration in some countries can take a few months, in others it can take many years!
Adriana lived a normal and happy life with both of her parents in Brazil. Sadly, 1 day, her mom was diagnosed with cancer of the kidneys. Her physical condition deteriorated quickly, with symptoms including weight loss, fever, and constant bone pain. The doctors, worried by her condition, could only administer Adriana’s mother a mediocre treatment. The best treatment, though available in the United States, was and is still not registered in Brazil. Because of this, all individuals in Brazil suffering from kidney cancer have no access to the best treatment, even though it is available in other parts of the world.
For you and your family to get access to the best treatment available for a disease, that product must first be registered in your country. If the pharmaceutical company behind the cancer kidney medicine had successfully registered the product in Brazil, Adriana’s mother would have received the best treatment available, increasing her chance of survival.
Accessibility
Even if a product has been successfully registered, can the patients access it? In developed countries, patients can rely on a strong system of hospitals, clinics, and pharmacies, which offer a wide range of medicines. To obtain the medicines, people can go by car or public transportation. Even better, in certain parts of the world, people can get their medicines delivered at home! However, not all countries have such strong healthcare systems in place.
For Akwasi, who suffers from diabetes and lives in a small, remote village north of Ghana, accessing the medicine he needs, insulin, can be a difficult task. The closest clinic is more than 60 kilometers away. Without public transportation or access to a car, reaching the closest clinic can be expensive and take a long time. Even worse, the clinic might not be equipped to provide the quality of care that Akwasi needs. Akwasi’s situation is not unique: around 44% of Ghana’s population lives in rural areas, where hospitals and clinics are not as numerous as in the cities2.
To ensure that patients receive the appropriate treatments even when they live in remote areas, such as islands or villages surrounded by jungles, pharmaceutical companies can develop strategies, such as partnering with drone companies to deliver its medicines (Figure 2). Furthermore, pharmaceutical companies can work to improve community-based care by improving the skills and confidence of healthcare workers. For example, companies can provide training to teach healthcare workers about the best way to use a new medicine to a patient in need.

- Figure 2 - Some companies are developing innovative techniques to reach isolated patients, such as using drones to deliver important medicines and vaccines!
Affordability
If you are lucky, you live in a country where the cost of your medicine is covered by your government. If so, that is great, because you will not have to spend your own money on important medication to treat your diseases. However, the government does not cover the cost of medicines in every country. For instance, in most low- and middle-income countries, home to most of the world’s poorest people, individuals are required to spend their own money to buy the medications they need. More precisely, in low-income countries, up to 70% of the money spent on medicines comes directly from the people who will use them [2]. Affordability thus becomes a key barrier to access.
Adils’ family, who lives in Morocco, must spend their own money for most of the medicines they need. Adil’s household makes about 500 € per month and this amount covers their basic needs, such as housing, food, and education. If Adil suddenly gets an infection like hepatitis C, the drug to treat this disease can easily cost more than the 500 € his parents make each month [3]. If such a situation happens, Adil’s family will have to make critical choices about how they spend their money, compromising on some expenses, such as food or education, to afford medicine.
Affordability is not just an issue in low-income countries. A recent drug therapy for a rare childhood disorder, spinal muscular atrophy, recently appeared on the market with a price tag of $2.1 million in the United States3. Would you or your family be able to afford this medicine?
To ensure affordability, companies need to assess people’s ability to pay. The price of a medicine should not be the same across the globe, because different populations have different incomes and expenses. One way to set affordable prices for medicines is to pay close attention to the factors in each country that affect people’s ability to pay, such as household income, education level, occupation, and more. That way, a medicine priced according to the population’s ability to pay in the United Kingdom will be priced differently in Morocco, so that people there can more easily afford it.
Acceptability
Although a drug is available, accessible, and affordable, there still might be a barrier to its use: acceptability. This refers to a patient’s ability and willingness to use a medicine. There are a number of factors that might affect how acceptable a medicine is, including how easy it is to take the medicine, as well as its size, shape, and color. Imagine if you had to inject yourself with a medicine every time you had a headache. Or swallow a syrup that tastes like broccoli when you have a cough. Would you do it? Of course not! This is part of what is meant by acceptability.
For Amina and her family, who live in Indonesia, religious and community leaders are respected figures who can influence the community’s willingness to use a specific medicine. The country’s main religion, Islam, sometimes requires certain items to be “halal,” for consumption. This halal label can also be required for vaccines and other medicines, and this label can affect the community’s acceptance. If a medical product is not halal, certain religious or community leaders might not support the product, and local communities might be reluctant to use it [4].
Pharmaceutical companies are expected to respond to community or population-specific concerns. They have the responsibility to understand the fears or worries of the patients and design their products with these in mind. While this can apply to the creation of halal medicines for the Muslim community, it also applies to many other situations and contexts, for example, making sure cough syrup tastes sweet enough that people will take it!
Conclusion
While the access-to-medicine issue is a topic that affects us all, individuals who are the most affected live in low- and middle-income countries. This is an inequality that should not be accepted as people all over the world should have equal access to good health. When developing new drugs, pharmaceutical companies should always be thinking about the 4As1. These companies have the power and money to make their medicines more available, accessible, affordable, and acceptable to people in need. If they take action to improve access to their medicines, no one will be left behind.
Glossary
Essential Medicines: ↑ Medicines that people should always have access to, in sufficient amounts, to stay healthy.
Diabetes: ↑ A disease in which blood sugar levels are too high. Without treatment, the disease can cause eye problems, vision loss, heart problems, and strokes.
Hepatitis C: ↑ A liver disease caused by a virus. The symptoms can range from fever to liver cancer.
Spinal Muscular Atrophy: ↑ A genetic disorder characterized by weakness and breakdown of the muscles used for movement.
Halal: ↑ An Arabic word from the Islamic religion, which indicates whether something is appropriate to consume or not, according to this religion.
Conflict of Interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
References
[1] ↑ Access to Medicine Foundation. 2018. Access to Medicine Index 2018. Access to Medicine Foundation. Available online at: https://accesstomedicinefoundation.org/access-to-medicine-index/2018-ranking
[2] ↑ Seale, A. C., Bianchi-Jassir, F., Russell, N. J., Kohli-Lynch, M., Tann, C. J., Hall, J., et al. 2017. Estimates of the burden of group B streptococcal disease worldwide for pregnant women, stillbirths, and children. Clin. Infect. Dis. 65:S200–19. doi: 10.1093/cid/cix664
[3] ↑ Hecht, R., Kaddar, M., Resch, S., El Kaim, J. L., Perfect, C., Sodqi, M., et al. 2019. Morocco investment case for hepatitis C: using analysis to drive the translation of political commitment to action. J. Glob. Health Rep. 3:e2019011. doi: 10.29392/joghr.3.e2019011
[4] ↑ Padmawati, R. S., Heywood, A., Sitaresmi, M. N., Atthobari, J., MacIntyre, C. R., Soenarto, Y., et al. 2019. Religious and community leaders’ acceptance of rotavirus vaccine introduction in Yogyakarta, Indonesia: a qualitative study. BMC Public Health 19:368. doi: 10.1186/s12889-019-6706-4
Footnotes
[1] ↑ http://www.uhc2030.org/fileadmin/uploads/uhc2030/Documents/Key_Issues/Private_Sector/UHC2030_Private_Sector_Constituency_Joint_Statement_on_UHC_FINAL.pdf.
[2] ↑ https://data.worldbank.org/indicator/SP.RUR.TOTL.ZS?locations=GH.
[3] ↑ https://www.statnews.com/2019/06/03/is-2-1-million-too-much-for-a-drug-for-affected-parents-there-is-no-debate/!
