Abstract
When you hear the word virus, you might think of diseases like rabies, influenza, or COVID-19. Viruses are organisms that must infect living cells to reproduce. Studies done on cells grown in the lab, called cell cultures, have contributed significantly to our understanding of viral diseases and to the development of treatments and vaccines. In the laboratory, cells can be grown in layers or in three-dimensional systems. By infecting cell cultures with viruses, scientists can study various aspects of the infection, such as how the virus gets into the cells or how the cells respond to infection. Knowledge gained from infecting cell cultures with viruses has helped scientists to vastly improve human health!
Introduction
Do you remember being sick with the flu, or maybe having a blister on your lip? You probably know that the flu is caused by the influenza virus, but did you know that lip blisters, often called cold sores or fever blisters, are also caused by a virus called herpes virus? Viruses are also responsible for diseases like measles, smallpox, COVID-19, and hepatitis. People are likely to become ill if they come into close contact with infected individuals or, in rare situations, animals.
The organism that is infected by a virus is called the host. Viruses infect the cells of various organs in the host’s body, such as the skin, lungs, or liver. Viral infection can cause our bodies to stop working properly, which makes us feel sick. Some viruses can be prevented by vaccines, and for certain viruses, doctors can give us medicines that help us to feel better. Have you ever wondered how scientists develop treatments and vaccines against viral diseases? To study viruses, scientists frequently grow cells from the human body in the laboratory, a process known as Cell culture [1]. Cell cultures can be infected with the virus scientists want to study, which can help them to learn a lot about a virus, including how to prevent or treat it.
What Are Viruses and Why Do They Infect Us?
Viruses are smaller and less complex than cells. They are primarily made up of a protein “shell” surrounding their genetic material (RNA or DNA). All the information required to make more viruses is encoded in their genetic material. Proteins perform several functions, including protecting the genetic material from the environment. Cells, on the other hand, have sophisticated machinery that allows them to make copies of their genetic material and to build proteins from it. Because viruses lack this machinery, they must infect cells before they can produce more viruses from their genetic material.
The ability of a certain virus to infect only specific cells, tissues, or animals is known as tropism. For example, the flu virus mostly affects the respiratory tract and only rarely attacks other organs. Certain features of the host’s cells or tissues, including the presence of proteins called receptors on the surface of cells, affect tropism. Viruses recognize and stick to certain receptors, like a lock and a key—this helps the viruses to get inside of certain cells. It is important to note that a key cannot open all locks, just like a virus cannot infect all cells—only the ones with the right receptor.
The genetic material of the virus can be read by the machinery of host cells, resulting in massive production of viral proteins and genetic material, which is used to assemble more viruses. In this way, an infected cell becomes a virus factory. The cell membrane eventually bursts, releasing new viruses to infect new cells. As a result, the virus spreads throughout the body (Figure 1).
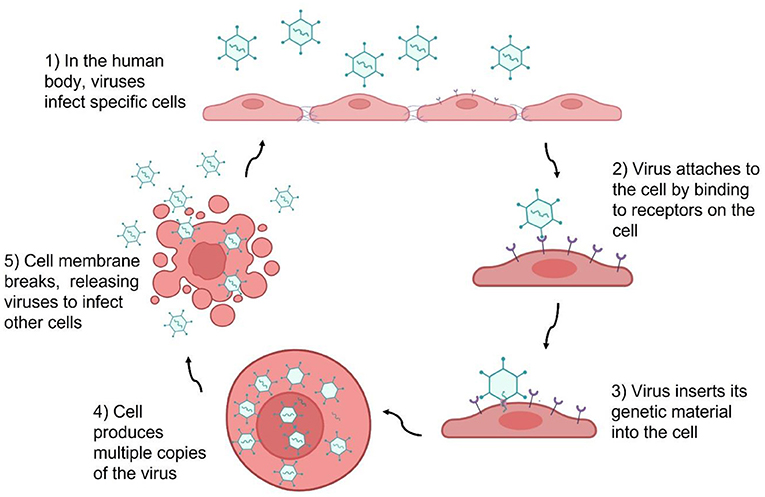
- Figure 1 - Viruses multiply within host cells.
- (1) Viruses enter the body and (2) infect specific cells by sticking to receptors on those cells. (3, 4) Once the virus’s genetic material is inside the cell, the cell makes many copies of the virus. (5) Eventually, the cell breaks open and viruses are released and can infect other cells.
Upon infection, host cells release specialized proteins that warn other cells, including those of the body’s defense system, that a virus is present. These protein signals prepare the body’s cells to fight infection. Infected people can spread viruses to others, for example, through saliva or blood. Some viruses can also persist for a short time on non-living surfaces like clothes or door handles.
Human Cells Can Be Grown in the Laboratory
Researchers can grow and study almost any type of cell in the laboratory, to understand its functions and behavior outside of the human body [2]. To accomplish this, a tissue sample must first be taken from a person and chopped up into smaller pieces. The tissue fragments are then treated with chemicals that break down the substances that surround the cells and hold them together. The cells are then spread out in a culture dish, or a special bottle called a tissue culture flask (Figure 2). Many cells die during the isolation procedure, but the cells that survive and attach to the plastic of the culture flask get most of the substances they need to grow from a nutrient-rich liquid called culture media, which scientists add to the cells. Cultures are typically incubated at 37°C, which resembles human body temperature. Cells are examined under the microscope daily to ensure they are in good condition and free of common contaminants like bacteria or yeasts. Some types of cells can now be purchased along with instructions for growing them in the lab.
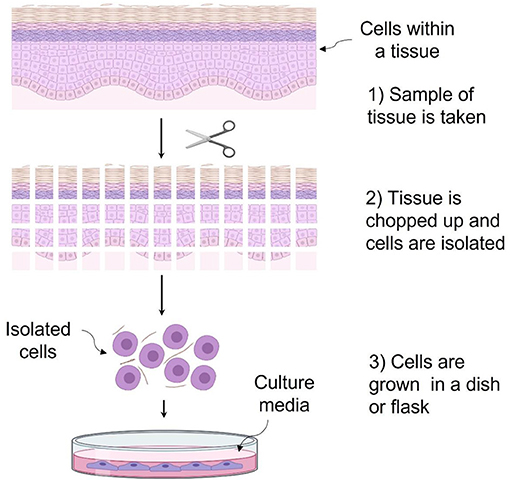
- Figure 2 - (1) To create a cell culture, a tissue sample is taken from a person.
- (2) Scissors and a scalpel are used to chop up the tissue sample. Chemicals are also added to help separate cells. (3) Once the cells are released from the tissue, they are placed in a culture dish or flask with some nutrient-rich culture media, at 37°C.
Cells cultured in the laboratory often grow by forming a thin sheet called a monolayer attached to the surface of the culture flask. However, to create an environment that is more like body tissues, three-dimensional (3D) cultures are often used. In a 3D culture, the cells grow inside a gel that can be made of various molecules (i.e., proteins) found in actual tissues [3]. These 3D cultures, known as hydrogels, behave more like actual tissues than monolayer cultures do, and they are also susceptible to viral infections.
Complicated 3D cultures called organoids, are generated from cells that can self-organize to mimic some characteristics of complex organs such as the liver, kidneys, lungs, or intestines. The organ-like structure of organoids improves viral tropism and increases the likelihood of viral infection.
In general, cell culture makes it possible to study multiple aspects of viral infection and to develop treatment strategies and vaccines.
How Do Scientists Study Viruses in the Laboratory?
Animals can also be used to study viruses in the lab. The choice to use animals or cell cultures depends on the type of virus being studied and the purpose of the study. For example, cell cultures are good for studying the multiplication of viruses. For SARS-CoV-2, the virus that causes COVID-19, the cell cultures allow researchers to study the type of cells that the virus can infect and the kind of damage the virus can cause to those cells. Researchers can also observe what happens when multiple viruses infect cells at the same time, as can happen when people are infected with both SARS-CoV-2 and influenza or hepatitis viruses.
Furthermore, infecting monolayer cell cultures allows scientists to produce vast quantities of viruses, for use in vaccine development or in the creation of treatments against viral diseases [4]. For example, poliovirus was one of the first viruses grown in cell culture and used to develop a vaccine. Poliovirus causes a dangerous disease called poliomyelitis, which, in severe cases, can result in paralysis of the legs, arms, and muscles that help control breathing. Thanks to cell culture, researchers can keep developing new vaccines, including some against SARS-CoV-2 [1].
3D cultures can be used to grow and study viruses to mimic infection in more realistic environment than in a monolayer. Organoid cultures grown from intestinal cells can be used to study the replication of rotavirus, a virus that causes severe diarrhea in infants. Also, brain organoids have been used to study Zika virus; this is important since Zika causes brain malformations in unborn babies when their mothers are infected with the virus. Virus such as papilloma, which cannot grow in monolayer cultures, have been successfully grown in 3D cultures. This virus is involved in the development of cervical cancer by infecting skin cells and even cells of the body’s defense system. 3D cultures can also help researchers to understand some of the communication strategies cells use to defend themselves against infection [5].
Cell Cultures Could Help Save Lives
Controlling viral diseases is one of the most important public health challenges that humanity faces. In this fight against viruses, cell cultures are an important tool for understanding the mechanisms by which viruses infect cells and cause disease. Cell cultures can also help researchers to develop vaccines and other treatments for viral infections. The next time you get a vaccine or visit the doctor for treatment of a viral illness, remember that cell cultures may have played a key part in the development of that treatment or vaccine.
Acknowledgments
The authors thank Professor Edgar Krötzsch for his comments and critical evaluation during the preparation of the manuscript.
Glossary
Host: ↑ Any organisms infected with a virus.
Cell Culture: ↑ Group of cells grown up into a culture dish in a laboratory.
Tropism: ↑ Ability of a virus to choose the right cell to multiply. A virus can infect several types of cells.
Receptor: ↑ Molecule produce by cell able to stick to viruses allowing them to enter the cell.
Culture Media: ↑ Mixture of nutrients, usually in liquid form, used to nourish cells.
Monolayer: ↑ Cells in a dish growing side by side to another filling all available surface in the dish.
Hydrogel: ↑ Polymer chains arranged in a three-dimensional network that can hold a lot of water.
Organoids: ↑ Cells grown in a dish able to organize in a similar way as complex organ.
Conflict of Interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
References
[1] ↑ Lawko, N., Plaskasovitis, C., Stokes, C., Abelseth, L., Fraser, I., Sharma, R., et al. 2021. 3D tissue models as an effective tool for studying viruses and vaccine development. Front. Mat. 80:631373. doi: 10.3389/fmats.2021.631373
[2] ↑ Noel, G., Baetz, N. W., Staab, J. F., Donowitz, M., Kovbasnjuk, O., Pasetti, M. F., et al. 2017. A primary human macrophage-enteroid co-culture model to investigate mucosal gut physiology and host-pathogen interactions. Sci. Rep. 7:45270. doi: 10.1038/srep45270
[3] ↑ Chopin-Doroteo, M., Salgado-Curiel, R. M., Pérez-González, J., Marín-Santibáñez, B. M., and Krötzsch E. 2018. Fibroblast populated collagen lattices exhibit opposite biophysical conditions by fibrin or hyaluronic acid supplementation. J. Mech. Behav. Biomed. Mater. 82:310–9. doi: 10.1016/j.jmbbm.2018.03.042
[4] ↑ Rijsbergen, L. C., van Dijk, L. L. A., Engel, M. F. M., de Vries, R. D., and de Swart, R. L. 2021. In vitro modelling of respiratory virus infections in human airway epithelial cells – a systematic review. Front. Immunol. 12:683002. doi: 10.3389/fimmu.2021.683002
[5] ↑ Geiser, J., Boivin, G., Huang, S., Constant, S., Kaiser, L., Tapparel, C., et al. 2021. RSV and HMPV Infections in 3D tissue cultures: Mechanisms involved in virus-host and virus-virus interactions. Viruses. 13:139. doi: 10.3390/v13010139
