Abstract
What is difficult about creating a new drug? In recent times, developing a new drug is based on understanding the specific processes of the disease the drug is meant to treat. However, this was not always the case. Drugs used to be discovered by a trial-and-error process, in which chemists tinkered with chemicals and hoped for success. How did we move from that inefficient method to the method we use today? Sir James Black is the father of two important medicines, propranolol (to treat high blood pressure) and cimetidine (to treat stomach ulcers). By focusing on what was causing those diseases, Black helped to transform drug development into the modern, efficient process we have today. How did a boy who came from a mining community in Scotland grow up to become the father of modern drug development? Keep reading to find out!
Introducing James Black
Taking medicines to relieve our symptoms or make us better is one of the most common things we do when we are sick. But did you ever stop to think about how new medicines are developed in the first place? The process is very different—and much more efficient—now than it used to be years ago!
Early drug development was based on the effects of natural products, such as using the natural pain-relieving properties of willow bark to develop aspirin. Back then, scientists did not have a deep understanding of how diseases developed. Therefore, figuring out whether a natural product worked against a certain disease was basically a process of trial and error—not a very efficient way to develop new medicines [1]! Over the years, scientists gained a better understanding of diseases, and that helped them to create new medicines that target specific pathways of the disease they are trying to treat [1]. Compared to older medicines, newer ones can provide patients with better treatment, with minimal side effects. But how did scientists get from a trial-and-error approach to specifically targeting disease pathways?
Enter, James Black
James Black grew up in a mining community in Fife, Scotland. Following his older brother, he studied medicine at the University of St. Andrews. After his graduation in 1946, he decided not to practice medicine and instead started his research career under Professor Robert C. Garry [2]. His research focused on investigating substances absorbed by the intestines and their effects on blood pressure. His time doing research had a positive impact on the rest of his career.
Black’s scientific journey was not a smooth one. He traveled the world for a few years and eventually became a lecturer in physiology in Singapore. While there, he continued to investigate the relationship between blood flow and absorption of medicines through the intestines. The unique cultures that Black encountered in Singapore helped him appreciate how different mindsets can lead to new methods of tackling problems.
Black returned to London in 1950 but had trouble finding a job. On one fateful day, he bumped into his old professor, Professor Garry, on Oxford Street on his way back from an interview [2]. To support his former student, Professor Garry arranged for Black to set up the Physiology Department at the University of Glasgow’s Veterinary School. As Black built the department, he also studied how a hormone called adrenaline affects the human heart. This paved the way for his future success, as you will soon see.
A Career Full of Twists and Turns
While at the University of Glasgow, Black built his career by turning his research ideas into medicines. However, his career took many twists and turns and was not considered the normal academic path. He switched between working for universities and drug-manufacturing companies several times, which helped him to build a bridge between the two areas.
One of the companies he worked for was called Imperial Chemical Industries, where he was highly successful. There, Black helped develop propranolol, a drug used to manage irregular heartbeats [2]. He later moved on to work as the head of biological research at SmithKline and French (now known as GlaxoSmithKline). While there, he investigated the effects of histamine, a substance involved in the immune response, and developed a medicine called cimetidine, which stops the production of stomach acid.
Black then switched back to academic research, accepting a position at University College London as a professor in pharmacology. But he missed working in industry, where it was easier to see the results of his research. Finally, he got his dream job King’s College London, where he was able to conduct academic research for industrial applications—the best of both worlds! Black’s path through both industry and academic research allowed him to build a remarkable career in drug development.
First Breakthrough—A Drug to Slow Down the Heart
Black’s focus on treating heart disease led to his first breakthrough in drug development—a medicine called propranolol [3]. Before propranolol was developed, treatment for heart diseases such as angina and high blood pressure were not always effective. Angina causes discomfort in the chest area, and high blood pressure can negatively affect multiple body systems. Individuals with high blood pressure are at a greater risk of heart failure.
Many bodily processes are controlled by chemicals called hormones. Adrenaline is a hormone that causes the heart to pump harder. To do so, it must stick to molecules called receptors on the surface of heart cells. Prior to this discovery, scientists did not know how adrenaline could cause the heart muscle to contract and relax. The American scientist Dr. Raymond Ahlquist was the first to suggest that the effects of adrenaline were controlled by two receptors, alpha and beta, that cause different responses in the heart muscle [3]. Black was strongly influenced by Ahlquist’s theory, and he worked on trying to decrease the workload of the heart.
At that time, heart disease was treated by increasing the amount of oxygen transported to the heart. In contrast, Black’s idea was to decrease the heart’s need for oxygen by making the heart work less hard. Beta blockers are medicines that reduce blood pressure by blocking the effects of the adrenaline (Figure 1). This causes the heart to beat more slowly and with less force, and opens veins and arteries to improve blood flow, which lowers blood pressure [4]. Black’s discovery completely changed the way doctors and researchers treated patients with heart disease, ultimately improving—and saving—many lives.
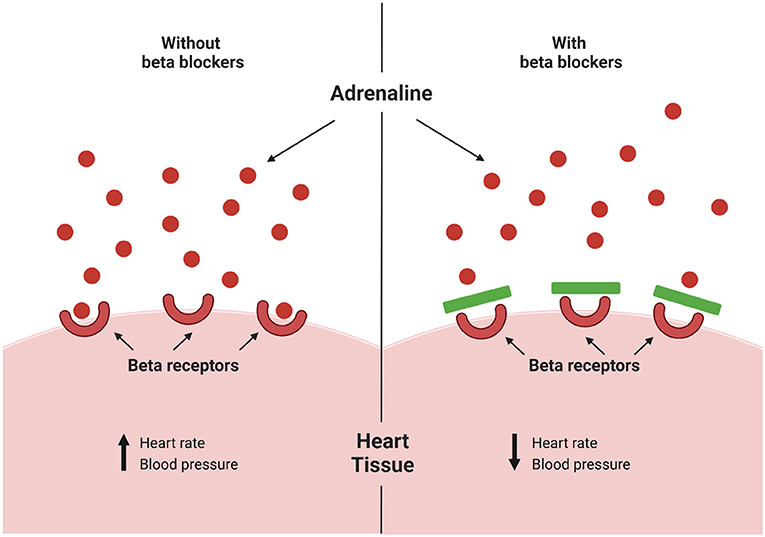
- Figure 1 - In the heart, the hormone adrenaline normally sticks to molecules called receptors on the surface of heart cells.
- One type of adrenaline receptor is called the beta receptor, and when adrenaline binds to this receptor it causes the heart to beat faster. Drugs called beta blockers (green bars) can block adrenaline from binding to the beta receptor, which decreases the workload of the heart and can help treat high blood pressure (Created with BioRender.com).
Second Breakthrough—A Drug to Reduce Stomach Ulcers
Black’s second groundbreaking discovery was a drug called cimetidine, which treats stomach ulcers [5]. Stomach ulcers are open sores in the lining of the stomach and the intestines. The stomach normally produces acid to help digest food and to kill dangerous bacteria. The stomach has a mucous lining to protect it from acid damage. Ulcers happen when the protective layer of mucus is reduced, which allows stomach acid to eat away the tissues that line the stomach. Increased stomach acid can also affect the esophagus, causing heartburn.
Limiting the production of acid can help to treat stomach ulcers, and Black worked closely with his team of scientists to find a medicine that could block the production of stomach acid. Acid-producing cells in the stomach, called parietal cells, have receptors on their surfaces for a chemical called histamine. When histamine binds to this receptor, it stimulates the parietal cells to produce acid. Black and his team identified the histamine receptor on parietal cells [5]. Cimetidine works by blocking histamine from binding to that receptor, stopping the acid-making parietal cells from responding to histamine, which decreases the production of stomach acid (Figure 2). This treatment can reduce the number and severity of stomach ulcers. The discovery of cimetidine helped to make stomach ulcers a treatable disease, rather than a disease that could reduce a person’s lifespan.
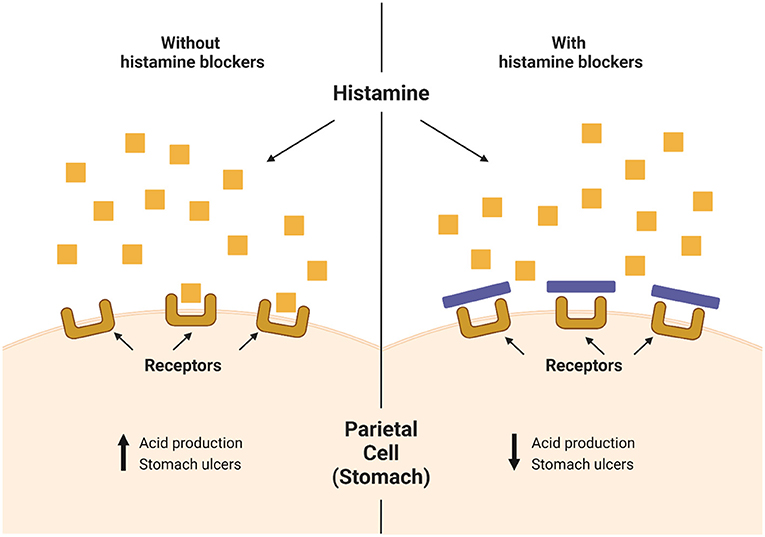
- Figure 2 - Parietal cells in the stomach normally secrete the stomach acid that digests food.
- Decreasing the amount of stomach acid produced is an effective way to treat ulcers. Normally, a chemical called histamine interacts with receptors on parietal cells and stimulates them to produce acid. Histamine blockers (purple bar) like cimetidine block histamine from attaching to those receptors, which decreases acid secretion (Created with BioRender.com).
Conclusion
The methods that Sir James Black used to create his medicines have changed drug development for the better. Propranolol and cimetidine revolutionized medical treatment of angina and stomach ulcers. Although these early medicines did have some side effects, his drug-development process helped other scientists to eventually create better medicines with fewer side effects. By providing knowledge about how receptors work and how to target them, Black helped to shape modern drug development.
Sir James Black’s passion, curiosity, determination, and perseverance are an inspiration for anyone trying to achieve their goals. The two medicines he developed were among the most important contributions to medicine and pharmacology in the 20th century. For his groundbreaking work in establishing the backbone of the modern drug-development process, Black won the Nobel Prize in Physiology or Medicine in 1988.
Glossary
Hormone: ↑ Chemical signals released by cells that control many of the body’s responses.
Adrenaline: ↑ A chemical that controls part of the body’s nervous system and is responsible for the fight or flight response, causing the heart to beat faster.
Propranolol: ↑ Medicine used to treat high blood pressure and prevent heart problems from getting worse. Part of the beta blocker class of medications.
Histamine: ↑ A chemical that is part of the body’s defense system and is also involved in the production of stomach acid.
Cimetidine: ↑ Medicine used to treat heart burn and stomach ulcers by stopping histamine activity in the stomach.
Receptors: ↑ Structures on the surfaces of cells that can turn certain cell functions on or off based on whether a molecule binds to them.
Beta Blocker: ↑ A class of medicines used to protect the heart by managing irregular heartbeats and blood pressure.
Parietal Cells: ↑ Cells located in the stomach that produce acid. Overactivity of these cells cause stomach issues like ulcers and heartburn.
Conflict of Interest
The authors declare that the research was conducted in the absence of any commercial or financial relationships that could be construed as a potential conflict of interest.
References
[1] ↑ Adam, M. 2005. Integrating research and development: the emergence of rational drug design in the pharmaceutical industry. Studies Hist. Philos. Sci. C. 36:513–537. doi: 10.1016/j.shpsc.2005.07.003
[2] ↑ Page, C. P., Schaffhausen, J., and Shankley, N. P. (2011). The scientific legacy of Sir James W. Black. Trends Pharmacol. Sci. 32:181–182. doi: 10.1016/j.tips.2011.02.009
[3] ↑ Stapleton M. P. 1997. Sir James Black and propranolol. The role of the basic sciences in the history of cardiovascular pharmacology. Texas Heart Inst. J. 24:336–342.
[4] ↑ Quirke V. 2006. Putting theory into practice: James Black, receptor theory and the development of the beta-blockers at ICI, 1958-1978. Med. Hist. 50:69–92. doi: 10.1017/s0025727300009455
[5] ↑ Molinder H. K. 1994. The development of cimetidine: 1964-1976. A human story. J. Clin. Gastroenterol. 19:248–254. doi: 10.1097/00004836-199410000-00017
