תַקצִיר
כל מי שיש לו אח או אחות צעירים מכיר את פלאי הפלסטר. איך ההדבקה של פלסטר על פצע יכולה לעשות פלאים לתחושת הכאב. אבל אנחנו יודעים שהפלסטר לא ממש משפיע על תחושת הכאב, הוא בסך הכל מכסה את הפצע. אז מדוע נראה שהפלסטר כל כך מקל על הכאב? הפלסטר הוא רק דוגמא אחת לתופעה רחבה יותר, תגובת הפלסבו. פלסבו היא תופעה כללית שבה מתן תרופת דֶמֶה לחולה, למשל כדור סוכר שנראה כמו תרופה, מפחיתה כאב ומביאה לשיפור משמעותי במחלה. כיצד זה קורה? היום אנחנו מבינים שמחשבות ורגשות יכולים להשפיע על האופן שבו הגוף שלנו מגיב לכאב, מחלה וטיפול. במאמר זה נדבר על תגובת הפלסבו, איך היא התגלתה, כיצד היא משפיעה על הרפואה וגם מה הבסיס הביולוגי מאחורי התופעה והאם נוכל לנצל אותו ואת פוטנציאל הריפוי שטמון בה כדי לייצר טיפולים יעילים יותר נגד מחלות רבות.
מהי תופעת הפלסבו (Placebo)?
אם תחפשו במילון את משמעות השם פלסבו, תגלו שהוא מתורגם לעברית במילים אין-בו. כלומר אין בו כלום. אבל אם אין בו כלום, למה הוא עושה כל כך הרבה רעש בתחום הרפואה, איך הוא משפיע על החולים וכיצד זה התחיל?
במהלך מלחמת העולם השנייה, חיילים שנפצעו בשדה הקרב סבלו מכאבים עזים מפציעותיהם. הטיפול שסופק על-ידי הצוותים הרפואיים היה משכך כאבים שמשתמשים בו עד היום ושמו ”מורפין“. באחד מימי המלחמה אזל מלאי המורפין לצוותים הרפואיים והחיילים נותרו בבית חולים ללא תרופה מתפתלים מכאבים. לצוות הרפואי לא הייתה דרך או יכולת להקל על סבלם של אותם חיילים, עד שלאחת האחיות צץ רעיון מבריק: היא אספה את המזרקים הריקים של המורפין, מילאה אותם במים (נטולי מורפין) והזריקה לחיילים הפצועים. באופן מפתיע לאחר ההזרקה של המים כאבם של החיילים נעלם!
עם תום המלחמה, אחד הרופאים שחזה במעשיה של האחות המבריקה, חזר לארצו והתחיל לחקור את נושא הפלסבו בצורה מעמיקה יותר, התוצאות היו מפתיעות! מסתבר שמחלות שונות משתפרות בעקבות קבלת תרופת הדֶמֶה (הפלסבו). כאב, למשל, מאוד מגיב לפלסבו. כמו הפלסטר לילדים כך תרופות-דֶמֶה, או טיפולי דֶמֶה, יכולים ממש להקל על הכאב. אפילו כאבים לאחר ניתוח, יכולים להשתפר מעצם מתן כדור דֶמֶה. מחלת הפרקינסון, בה אנשים סובלים מרעד בלתי נשלט בגופם, משתפרת מאוד כאשר נותנים לחולים כדור דֶמֶה. אנשים שחולים באסטמה ואלרגיות מגיבים היטב לכדורי סוכר או למשאפים שאין בהם כל תרופה. ישנם אפילו ניתוחי פלסבו בהם החולה מוכנס לחדר ניתוח, מורדם, לפעמים אפילו מבצעים לו חתך בעור, אבל בפועל, לא נוגעים בשום איבר פנימי. מדהים לראות כיצד מצבם של חולים מסוימים ממש משתפר בעקבות ניתוחי הדֶמֶה הללו [1].
חוקרים רבים ניסו לבחון את ההשפעה הפסיכולוגית של הפלסבו וגילו, למשל, שלגודל הכדור (התרופה) שנותנים לחולה יש השפעה גדולה על מידת התגובה שלו לטיפול. אם נותנים לחולה כדור גדול או כדור קטן, הכדור הגדול יהיה יותר יעיל למרות ששניהם בסך-הכל מכילים רק סוכר. גם לצבע של הכדור יש משמעות. לכדורים בצבעים שונים - השפעה שונה. למשל, כדור אדום יוצר תופעות והשפעות שונות מאשר כדור כחול וכמובן, אחד הדברים שהכי משפיעים על יעלות הטיפול, הוא מחיר התרופה. ככל שהתרופה יקרה יותר היא יעילה יותר [2].
השימוש בפלסבו מעורר שאלות מוסריות רבות. מצד אחד, האם על-ידי מתן תרופת דֶמֶה הרופא מרמה את החולה? אבל, מאידך הוא עוזר למטופל בכך שהוא משפר את מצבו מבלי לתת לו חומרים כימיים שגם להם יש תופעות לוואי. האם לא מחובתו של הרופא קודם כל לא להזיק ולרפא כמיטב יכולתו? השימוש בפלסבו כה נפוץ במספר מדינות, בייחוד בגרמניה, עד שהשאלה הפכה לשאלה משפטית ואתית סבוכה.
לסיכום, פלסבו הינה תופעה כללית שבה מתן תרופת דֶמֶה לחולה מפחיתה את כאבו, משפרת את מצבו וגורמת לשיפור במצבו הרפואי (אם כי לפעמים ההשפעה של הטיפול היא פחותה או קצרת מועד יחסית לטיפול אמיתי). היכולת של תרופת הדֶמֶה הזו לרפא מחלות מרתקת מדענים מזה שנים. תופעה זו הייתה ונותרה אחת התעלומות הגדולות של המדע, והיא המחשה נוספת לצורה בה מחשבות ורגשות יכולים להשפיע על המצב הבריאותי שלנו. קיומו של אפקט הפלסבו אינו מוטל בספק, אבל המנגנון בו אותן תרופות דֶמֶה תורמות לשיפור בריאות האדם לא פוענח במלואו עד היום.
איך זה קורה?
כדי להבין לפחות חלקית, את מה שקורה, נחזור לפלסטר.
כידוע לנו (ולכם 😊) שני דברים מאפיינים ילדים – הדבר הראשון הוא שיש להם זיכרון טוב, והשני הוא העובדה שהם נפצעים באופן תדיר. הילד זוכר שבפעם הראשונה בה הוא נפצע, שמו לו פלסטר ואמרו לו שהכול יעבור. אחרי תקופה מסוימת, הפצע הגליד והכאב נעלם כחלק מתהליך הריפוי הטבעי. למרות שהפלסטר לא משפיע על תחושת הכאב, מה שנחרט בזיכרונו של הילד זה שהכאב נעלם בעקבות הדבקת הפלסטר. כך הילד מחבר במוח ויוצר התניה (יצירת קשר ותלות בין שני דברים) בין הפלסטר לתחושת ההקלה בכאב.
מהי התניה?
המחקר הבסיסי לגבי התניות מיוחס למדען רוסי בשם פבלוב (Pavlov). כאשר אנחנו אוכלים, הגוף שלנו מגיב בצורות שונות: ריר מופרש מהפה כדי להקל בלעיסה ובליעה, חומצות מופרשות בקיבה כדי לפרק את המזון וכדומה. זה היה תחום עניינו של פבלוב: הוא חקר איך הגוף מגיב לאוכל. כפי שקורה פעמים רבות במדע, תוצאות לא צפויות של ניסויים מובילות לתגליות מרתקות. פבלוב חקר כלבים ובכל בוקר כאשר הוא הגיש להם את האוכל, הוא צלצל בפעמון כדי לקרוא להם. אחרי שהם אכלו, הוא בחן תגובות שונות של מערכת העיכול שלהם. למשל מתי הם החלו להזיל ריר. לאט לאט הוא הבחין שהכלבים לא היו צריכים לקבל את האוכל כדי להתחיל להזיל ריר, זה קרה כבר כשצלצל בפעמון, אפילו אם לא הגיש להם אוכל. מדוע? הכלבים התרגלו לכך שצלצול בפעמון שקוּל לאוכל. כאשר הם שמעו צלצול את הפעמון, הם חשבו וציפו שיקבלו אוכל וזה גרם לגופם להגיב בהתאם (איור 1). בניסוי זה, פבלוב למעשה הראה איך מחשבות וציפיות יכולות להשפיע על הגוף אצל כלבים. כך גם אנחנו, בני האדם, מגיבים בצורה דומה (מי מאתנו לא החל להזיל ריר בהישמע צלצול הפעמון של שליח הפיצה בדלת?) [3].
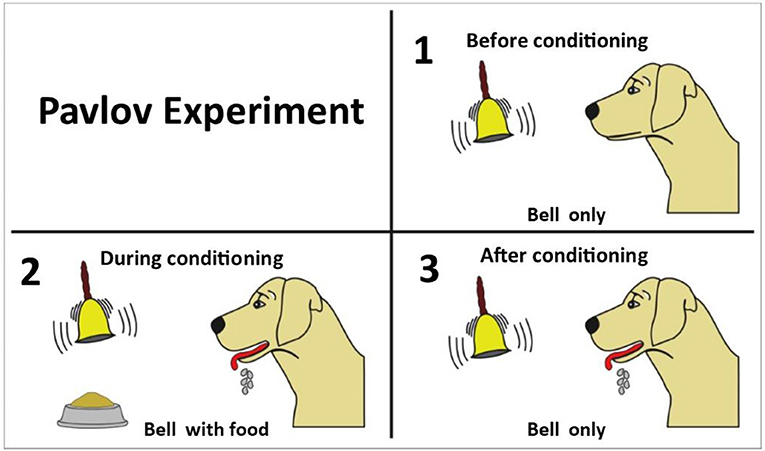
- איור 1 - הניסוי של פבלוב.
- 1) לפני ההתניה, הכלבים הגיבו בהזלת ריר כאשר הם ראו אוכל, ואילו צלצול הפעמון לבד לא גרם לתגובה מסוימת אצל הכלבים. 2) במהלך ההתניה, פבלוב צלצל בפעמון בכל פעם שהוא הגיש אוכל לכלבים. 3) אחרי ההתניה, צלצול הפעמון לבד גרם להזלת ריר אצל הכלבים, גם אם לא הוגש להם אוכל.
בדומה למה שקרה בניסוי של פבלוב עם הכלבים, החיילים הפצועים, חשבו שהם מקבלים מורפין (משכך הכאבים), לכן הם ציפו שהכאב שלהם יפחת וכך למרות שלזריקות המים (נטולות המורפין) אין את היכולת לשכך כאב, עצם המחשבה שיככה את הכאב.
אבל זה לא הכל, רופאים גילו כי גם במקרים בהם המטופל מקבל תרופה שלא נחשף אליה בעבר. כלומר, לחולה לא היה אירוע דומה בעבר שיכול לקשר אותו עם החוויה הנוכחית ואין התניה כמו במקרה עם הפלסטר, אפקט הפלסבו עדיין נוכח והוא יכול לשפר את מצבו של החולה ולתרום לריפוי המחלה. מה קורה במקרה כזה?
פה נכנס רכיב אחר, הציפייה. כאשר חולה מקבל תרופה, גם אם היא חדשה לו, זה מעורר אצלו מחשבות חיוביות וציפייה לשיפור במצבו. ההשערה היא שעצם המחשבה החיובית והציפייה לריפוי תורמות להקלה בכאב, שיפור המצב וריפוי.
המוח ומערכת החיסון
כידוע לנו, המוח הוא זה ששולט במחשבות ובציפיות שלנו. מערכת החיסון היא אחת המערכות החשובות לשמירה על המצב הבריאותי שלנו והיא מתפקדת כמו צבא אשר מורכב ממספר גדול מאוד של תאים שונים אשר פועלים יחדיו כדי להתגבר על מחלות ולשמור על גוף בריא ותקין.
במעבדתנו רצינו להבין כיצד התהליכים הללו מתרחשים, כיצד בדיוק המוח יכול להשפיע על מערכת החיסון? זה חשוב משום שרק אם נבין איך דברים עובדים נוכל להשתמש בידע הזה לריפוי מחלות ופיתוח תרופות.
המדע כיום יודע לאפיין אזורים במוח המעורבים בתפקידים שונים, כך הוכח כי עצם הציפייה של חולה לשיפור במצבו מפעילה תאים ואזורים במוח אשר מהווים חלק מרשת שנקראת מערכת התגמול. השאלה היא, האם ההפעלה של אזורים אלה יכולה להשפיע על תהליכי ריפוי של הגוף.
במחקר שלנו ניסינו לדמוֺת את תהליך הפלסבו בחיות מעבדה (עכברים). בשלב הראשון, הזרקנו, בצורה מאוד מדויקת, מעין ״מְתָגִים״ (חומר ביולוגי שנכנס לתאי עצב ומאפשר לנו לשלוט בפעילות של אותם תאים) להפעלה וכיבוי של תאי עצב של מערכת התגמול במוח. זה אִפשר לנו להפעיל כמו בשלט רחוק את מערכת התגמול. במידה רבה, הפעלה כזו מדמה את מה שקורה במוח בעת ציפייה חיובית, כמו שקורה גם בתגובת הפלסבו. ראינו כי ההפעלה של אותם אזורים שאחראיים על רגשות חיוביים וציפייה לריפוי גרמה להפעלה של מערכת החיסון ושיפור היכולת שלה להתמודד עם מחלות. למשל, גילינו שבעקבות ההפעלה של מערכת התגמול במוח, תאי מערכת החיסון יכלו לחסל חיידקים בצורה יעילה יותר ולהתמודד עם מחלה בצורה יעילה. מכאן הסקנו שהפעלת מערכת התגמול במוח גורמת לכך שמערכת החיסון תפעל בצורה יעילה יותר במלחמתה נגד חיידקים [4] (איור 2).
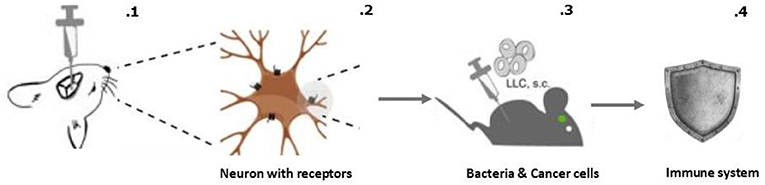
- איור 2 - הפעלה של מערכת התגמול במוח גרמה לשיפור פעילות מערכת החיסון נגד חיידקים ותאים סרטניים.
- 1) הזרקנו בצורה מדויקת מְתָגִים לאזור מערכת התגמול במוחות של העכברים. 2) המתגים חדרו לתאי העצב של מערכת התגמול מה שאִפשר לנו לשלוט בהפעלה של אותם תאים. 3) אחר כך, אתגרנו את מערכת החיסון של העכברים על-ידי חיידקים ותאים סרטניים. 4) ראינו שהפעלת מערכת התגמול גורמת לכך שמערכת החיסון תפעל בצורה יעילה יותר במלחמתה נגד חיידקים ותאים סרטניים.
תפקיד חשוב נוסף של מערכת החיסון הוא להילחם בסרטן ובמחלות ממאירות. לכן, אם ההפעלה של מערכת התגמול במוח הגבירה את היכולת של מערכת החיסון להילחם בחיידקים, רצינו לבדוק אם היא תוכל להגביר גם את היכולת של מערכת החיסון להילחם בסרטן. לשם כך, אתגרנו את מערכת החיסון של העכברים על-ידי תאים סרטניים והפעלנו את מערכת התגמול במוח. בדומה למקרה עם החיידקים, גם כאן אחרי שהפעלנו את מערכת התגמול במוח, מערכת החיסון פעלה בצורה יעילה יותר וחיסלה יותר תאים סרטניים [5] (איור 2).
השאלה הבאה שעמדה בפנינו הייתה להבין כיצד תִקשרה מערכת התגמול במוח עם מערכת החיסון שנמצאת באיברים שונים בגוף ולעיתים מאד רחוקה מהמוח. בגופנו ישנה ”מערכת חירום“, הנקראת המערכת הַסִּימְפָּתֶטִית שהיא חלק ממערכת העצבים הכללית בגוף. מערכת זו נכנסת לפעולה בדרך כלל כאשר הגוף שלנו צריך להתמודד עם מצוקה, מחלה למשל. המערכת הזו מכילה מעין חוטי עצבים שמחברים בין המוח לשאר האיברים והמערכות בגוף, כגון מערכת הלב, מערכת העיכול וגם מערכת החיסון. לכן, הפעילות של המערכת הסימפתטית יכולה להשפיע על פעילותם של איברים שונים בגוף. דוגמא לכך היא ההגברה של קצב הלב כאשר אנחנו רצים או מתאמצים. באופן דומה, מצאנו כי ההפעלה של מערכת התגמול השפיעה על אותה ”מערכת חירום“, המערכת הסימפתטית, וזו השפיעה על תאי מערכת החיסון להיות ״לוחמניים״ יותר כלפי הגידול הסרטני. כיצד היא עשתה זאת? [4, 5]
כדי להתאים את עצמם לאתגרים שעומדים בפניהם, תאי מערכת החיסון צריכים להתחדש כל הזמן. למשל, בעת פלישה חיידקית, יש צורך להגדיל את כמות תאי מערכת החיסון. לכן, קיים מאגר של תאי מערכת החיסון ובו תאי גזע. תאי הגזע הם תאים שיכולים לייצר את כל מגוון תאי מערכת החיסון בגופנו. תאי הגזע הללו יושבים בעצמות. במרכז העצם ישנו חלל אשר מלא בתאי גזע של מערכת החיסון שנקרא ”מֵחַ העצם.“ מסתבר, שהחוטים העצביים של מערכת העצבים הסימפתטית, עליה דיברנו קודם, יוצאים מהמוח ומגיעים גם לעצמות, בדיוק למקום בו יושבים תאי הגזע ושמיוצרים בו תאי מערכת החיסון. שם, אותם חוטים יכולים להשפיע על האופן שבו תאי מערכת החיסון מיוצרים ומתפתחים (איור 3). לכן, כאשר הפעלנו את מערכת התגמול במוח, היא השפיעה על פעולת מערכת העצבים הסימפתטית וזו בתורה, השפיעה על כך שתאי מערכת החיסון החדשים שנוצרו במח העצם, היו לוחמניים יותר ויעילים יותר נגד תאי הסרטן, והצליחו לצמצם את גודלם של גידולים סרטניים [5]. כלומר, אפשר לסכם כי תאי גזע זה כמו מחלקות בצבא. יש חיילים שלמדו להילחם רק נגד אויבים מסוימים. תאי גזע הם הלוחמים החדשים, שעדיין לא התאמנו והם יכולים ללמוד להילחם במי שהם רוצים. מוח העצם הוא המחנה ומערכת העצבים היא המפקד של הצבא, שמשפיע על התפקוד של תאי מערכת החיסון החדשים.
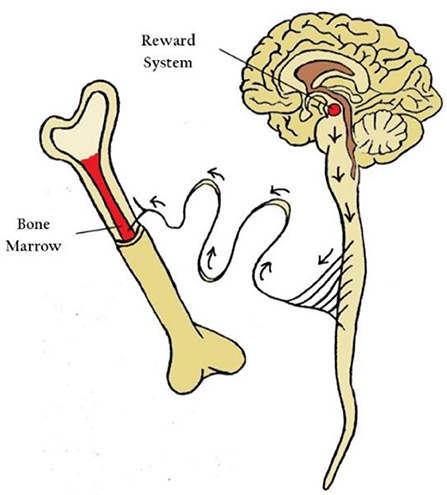
- איור 3 - הפעלה של מערכת התגמול במוח משפיעה על פעילות מערכת העצבים בגוף, חוטים של מערכת העצבים מגיעים למח העצם (מקום ייצור תאי מערכת החיסון), מה שמוביל לייצור תאי מערכת חיסון יותר ”לוחמניים“ בעקבות הפעלה של מערכת התגמול.
לסיכום
זהו אחד המחקרים המדעיים הראשונים שמציעים הסבר לדרך בה מחשבות ורגשות יכולים להשפיע על מערכת החיסון והמצב הבריאותי שלנו. מחקר כזה פותח צוהר חדש לטיפול במחלות. בעקבותיו, אפשר לנסות לשלב טכנולוגיות חדשות שמאפשרות לנו להפעיל אזורים שונים במוח, ובכך להשפיע על מהלכן של מחלות. בשנים האחרונות התפתחו טכנולוגיות רבות שמאפשרות לנו לשלוט על פעילות המוח, למשל על-ידי קסדות מיוחדות שמייצרות שדה מגנטי אשר מכוון לאזור מסוים במוח וכך יכולות לשלוט על פעילותו. ישנם אפילו משחקי מחשב מיוחדים שמיועדים לגרום לאדם להפעיל אזורים מסוימים במוח בצורה ספציפית.
חשוב לזכור שהמחקר הזה שלנו הוא רק קצה הקרחון. כאשר אנו חווים חוויה מסוימת, מרגישים רגש או חושבים מחשבה, מופעלים הרבה מאד דברים במוח ובגוף שאת רובם אנחנו עדיין לא מבינים. אצל כל אחד מאתנו, חוויות שונות מפעילות את המוח בצורה שונה ולא כל האנשים מגיבים לפלסבו באותה צורה. לכן, עוד ארוכה הדרך עד שנפענח את המנגנונים העומדים בבסיס אפקט הפלסבו. אבל בינתיים נראה שהמשפט ”הכל בראש“ אינו רק קלישאה, אלא משפט עם ביסוס מדעי והשפעות מרחיקות לכת על גופנו ובריאותנו.
מילון מונחים
מערכת החיסון: ↑ מערכת שיטור מתוחכמת ביותר, היא פועלת בכל רחבי הגוף ומחפשת אחרי פולשים בגופנו (כמו: וירוסים, חיידקים ותאי סרטן) ונלחמת נגדם.
מערכת התגמול: ↑ רשת של תאים עצביים ומבנים שנמצאים במוח, אשר יוצרים תחושה של עונג בתגובה לגירויים מסוימים. התאים במערכת הזו מְתַקְשֵרים זה עם זה דרך חומר שנקרא ”דּוֹפָּמִין“ והוא זה שיוצר את תחושת העונג.
המערכת הַסִּימְפָּתֶטִית: ↑ מערכת החירום ששולטת בגופנו. היא מתווכת תגובה שנקראת ”הילחם או ברח", וכפי ששמה מעיד היא פועלת במצבי מצוקה, כמו: לברוח מאויב או להילחם במחלה. מערכת זו משפיעה של פעילותן של מערכות אחרות בגופנו כמו: מערכת הלב, מערכת העיכול וגם מערכת החיסון.
תאי גזע: ↑ תאים מיוחדים שאינם מחויבים להתפתח לסוג איבר מסוים ויש להם פוטנציאל להתפתח ולהפוך לסוגי תאים רבים.
מֵחַ העצם: ↑ חלל שנמצא בתוך העצמות, בתוכו מתיישבים תאי הגזע אשר מהם מתפתחים תאי מערכת החיסון שלנו.
הצהרת ניגוד אינטרסים
המחברים מצהירים כי המחקר נערך בהעדר כל קשר מסחרי או פיננסי שיכול להתפרש כניגוד אינטרסים פוטנציאלי.
תודות
אנו מודים לדוקטורנטית מריה קרוט על ציור האיורים במאמר ועריכתם.
מאמר המקור
↑ Ben-Shaanan, T. L., Azulay-Debby, H., Dubovik, T., Starosvetsky, E., Korin, B., Schiller, M., et al. 2016. Activation of the reward system boosts innate and adaptive immunity. Nat. Med. 22:940–4. doi: 10.1038/nm.4133
מקורות
[1] ↑ Beecher, H. K. 1955. The powerful placebo. J. Am. Med. Assoc. 159:1602–6.
[2] ↑ Rajagopal, S. 2006. The placebo effect. Psychiatr. Bull. 30:185–8. doi: 10.1192/pb.30.5.185
[3] ↑ Pavlov, I. P., and Anrep, G. V. 1928. Conditioned reflexes: An investigation of the physiological activity of the cerebral cortex. London: Oxford University Press.
[4] ↑ Ben-Shaanan, T. L., Azulay-Debby, H., Dubovik, T., Starosvetsky, E., Korin, B., Schiller, M., et al. 2016. Activation of the reward system boosts innate and adaptive immunity. Nat. Med. 22:940–4. doi: 10.1038/nm.4133
[5] ↑ Ben-Shaanan, T. L., Schiller, M., Azulay-Debby, H., Korin, B., Boshnak, N., Koren, T., et al. 2018. Modulation of anti-tumor immunity by the brain’s reward system. Nat. commun. 9:2723. doi: 10.1038/s41467-018-05283-5
